If you have ever submitted a CHF claim and watched it bounce back with a denial, you already know the pain. You did the work. The patient was seen. The notes were written. But still — rejected. Most of the time, the problem is not your effort. The problem is the code. Specifically, it is using a vague or wrong DX code for CHF ICD-10 when a more precise one was right there waiting.
This guide breaks down every ICD-10 code you need for congestive heart failure in 2026, why specificity matters more than ever, and exactly how to stop leaving money on the table.
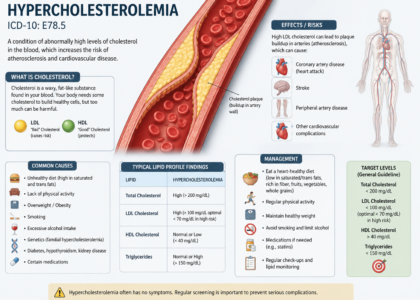
What Is the DX Code for CHF ICD-10 in 2026?
Let’s get straight to it. The primary diagnosis code family for congestive heart failure in ICD-10-CM is I50, which falls under Chapter 9 — Diseases of the Circulatory System. However, just using I50 alone will get your claim denied faster than you can say “prior auth.”
The root code I50 is a non-billable, non-specific parent code. Think of it as an umbrella. You need to go deeper — to the specific subcategories — to actually bill and get reimbursed.
Here is what the 2026 ICD-10-CM I50 family looks like:
| ICD-10 Code | Description |
|---|---|
| I50.1 | Left ventricular failure, unspecified |
| I50.20 | Unspecified systolic (congestive) heart failure |
| I50.21 | Acute systolic (congestive) heart failure |
| I50.22 | Chronic systolic (congestive) heart failure |
| I50.23 | Acute on chronic systolic (congestive) heart failure |
| I50.30 | Unspecified diastolic (congestive) heart failure |
| I50.31 | Acute diastolic (congestive) heart failure |
| I50.32 | Chronic diastolic (congestive) heart failure |
| I50.33 | Acute on chronic diastolic (congestive) heart failure |
| I50.40 | Unspecified combined systolic and diastolic heart failure |
| I50.41 | Acute combined systolic and diastolic heart failure |
| I50.42 | Chronic combined systolic and diastolic heart failure |
| I50.43 | Acute on chronic combined systolic and diastolic heart failure |
| I50.810 | Right heart failure, unspecified |
| I50.814 | Right heart failure due to left heart failure |
| I50.9 | Heart failure, unspecified |
That last one — I50.9 — is the killer. It is the code most beginner coders default to, and it is also the one that triggers the most payer audits and medical necessity denials. Avoid it whenever the documentation gives you anything more specific to work with.
Why CHF Coding Specificity Is a Big Deal in 2026
Here is the truth that nobody talks about enough: payers in 2026 are smarter and more aggressive about audits than ever before. Medicare Advantage plans, in particular, run algorithm-based claim scrubbers that flag generic CHF codes almost instantly.
When you submit I50.9 on a claim, you are essentially telling the payer: “We don’t really know what type of heart failure this patient has.” That alone raises red flags. Payers want to see that the documentation supports a specific clinical picture — type, acuity, and cause.
Furthermore, for risk adjustment under Hierarchical Condition Category (HCC) coding, CHF falls under HCC 85. To properly capture risk-adjusted revenue for Medicare Advantage patients, coders need a specific and well-documented CHF ICD-10 code. Vague entries simply do not score in risk-adjustment models, which means your practice loses capitation dollars on top of individual claim denials.
So, specificity is not just a compliance checkbox. It directly affects your revenue.
Breaking Down the Two Main CHF Types You Must Know
Before you pick a code, you have to understand what you are coding. Congestive heart failure comes in two primary flavors, and they bill differently.
Systolic Heart Failure (HFrEF) — Codes I50.2x
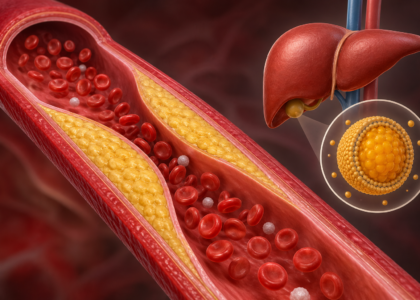
Systolic CHF, also called Heart Failure with Reduced Ejection Fraction (HFrEF), happens when the heart muscle is too weak to pump blood out effectively. The ejection fraction (EF) is typically 40% or below. This is the “pump failure” type.
- I50.21 — Acute systolic CHF: Sudden onset, patient presenting in decompensation
- I50.22 — Chronic systolic CHF: Long-standing, stable pump dysfunction
- I50.23 — Acute on chronic systolic CHF: A chronic patient who just got significantly worse
Diastolic Heart Failure (HFpEF) — Codes I50.3x
Diastolic CHF, or Heart Failure with Preserved Ejection Fraction (HFpEF), is the sneaky one. The heart pumps fine, but the ventricle is stiff and cannot relax properly to fill up with blood. EF is typically above 50%.
- I50.31 — Acute diastolic CHF
- I50.32 — Chronic diastolic CHF
- I50.33 — Acute on chronic diastolic CHF
Combined Systolic and Diastolic — Codes I50.4x
Some patients have both problems happening at the same time. When documentation clearly supports both types, you move into the I50.4x range, which requires solid clinical backing from echo reports or provider notes.
Coding CHF with Hypertension: The Sequencing Trap
One of the most common — and costly — coding errors involves CHF patients who also have hypertension. A lot of coders just stack both diagnoses without thinking about sequencing. That is a mistake.
When a patient has both hypertensive heart disease and heart failure, ICD-10-CM requires you to use a combination code first. Specifically, you should be using I11.0 (Hypertensive heart disease with heart failure) as the primary code, and then adding the appropriate I50 code to specify the type of heart failure.
Using a standalone I50 code when hypertension is present and documented as causally related is a sequencing error. It can trigger a denial and is also a compliance risk during audits.
Similarly, if the patient has both hypertension and chronic kidney disease contributing to heart failure, you will want to look at the I13.x combination codes, which capture all three conditions together.
What Documentation Must Say for Clean CHF Claims
Great coding starts with great documentation. As a coder, you cannot pull a specific CHF code out of thin air — the provider has to document it clearly. Here is exactly what needs to appear in the chart to support a specific DX code for CHF ICD-10:
The Three Must-Have Elements:
- Type — Is it systolic, diastolic, or combined? The provider should state this explicitly or document an ejection fraction that makes it clear.
- Acuity — Is this an acute presentation, a chronic condition, or an acute exacerbation of a chronic condition (acute-on-chronic)? This distinction alone changes the code you use.
- Cause or Contributing Factor — Is hypertension driving it? Is there a valve problem, coronary artery disease, or alcohol-related cardiomyopathy involved? Linking cause to code strengthens your claim and improves risk-adjustment accuracy.
When documentation says nothing more than “CHF,” the coder is stuck with I50.9. That puts your practice at risk. The practical fix is a simple physician query process — asking the provider to clarify type and acuity when it is not obvious in the notes. This one habit alone can dramatically improve your clean claim rate.
The Top CHF Coding Mistakes That Cause Denials
Let’s be real here. These are the errors that show up again and again in billing audits, and they are all avoidable.
Using I50.9 when you have enough info to go specific. If the echo is in the chart and it shows an EF of 35%, there is no reason to leave it at “unspecified.”
Forgetting to sequence hypertension first. When CHF and hypertension are linked, I11.0 comes before the I50 code. Every time.
Skipping the acuity distinction. Acute, chronic, and acute-on-chronic are completely different clinical realities. Payers know this, and they will flag a claim that bills chronic coding for a patient presenting in acute decompensation.
Not querying the physician. If the notes are vague, do not guess. Send a query. Document the response. Then code from that.
Missing right heart failure codes. The I50.81x codes specifically cover right-sided heart failure. If your provider documents right heart failure due to left heart failure, I50.814 is your code — not a generic I50.9.
2026 Updates That Actually Affect CHF Coding
The 2026 ICD-10-CM updates that went live on October 1, 2025 continue the trend of demanding greater specificity across cardiac diagnoses. The April 1, 2026 quarterly update files from CMS also reinforced proper code usage for complex comorbid presentations.
The key takeaway from 2026 guidelines is this: payers and CMS are tightening validation on heart failure claims, especially for Medicare Advantage and risk-adjusted populations. Practices that have not updated their internal CDI (Clinical Documentation Integrity) workflows are going to feel this in their denial rates throughout the year.
Additionally, if your practice bills for Chronic Care Management (CPT 99490), CHF is one of the qualifying chronic conditions — but only if the ICD-10 codes tied to that billing are specific and properly documented. Throwing a generic I50.9 onto a CCM claim is a fast path to a denial and a potential compliance headache.
Quick Reference: Choosing the Right CHF Code Every Time
Follow this simple decision tree before you submit any CHF claim:
Step 1: Does documentation confirm systolic or diastolic dysfunction? Go to I50.2x or I50.3x.
Step 2: Is the presentation acute, chronic, or acute-on-chronic? Pick the matching fourth digit.
Step 3: Is hypertension listed as a cause? Use I11.0 first, then add the I50 specificity code.
Step 4: Is right heart failure present? Consider I50.810 or I50.814.
Step 5: Still not sure? Send a physician query before you code. Do not default to I50.9 if you can avoid it.
FAQs
Q: What is the most specific ICD-10 code for CHF in 2026?
A: It depends on the patient’s documented type and acuity. For example, I50.23 covers acute-on-chronic systolic CHF, while I50.33 covers acute-on-chronic diastolic CHF. These are among the most specific billable codes in the I50 family.
Q: Can I use I50.9 at all?
A: Yes, but only when documentation truly does not support anything more specific. Use it as a last resort, not a default. Overusing I50.9 is a known audit trigger.
Q: What is the DX code for CHF with hypertension?
A: Use I11.0 as the primary code for hypertensive heart disease with heart failure, followed by the appropriate I50 subcategory code for the type and acuity of the heart failure.
Q: Is congestive heart failure the same as systolic heart failure in ICD-10?
A: Not exactly. “Congestive” is a clinical description that can apply to both systolic and diastolic types. In ICD-10, you still need to specify which type is present. I50.9 captures unspecified heart failure but should never be your go-to code when more detail is available.
Q: What happens if I sequence CHF before hypertension?
A: You risk a claim denial and a compliance flag. When both conditions are present and linked, hypertension (I11.0) must be sequenced first per ICD-10-CM coding conventions.
Q: Does CHF qualify for Chronic Care Management billing?
A: Yes. CHF is a qualifying chronic condition for CPT 99490, but the diagnosis code supporting the CCM billing must be specific and well-documented. A generic I50.9 weakens the claim.
Q: How often do CHF codes get updated?
A: ICD-10-CM is updated annually on October 1, with a possible mid-year update on April 1. Always check the current CMS code files to make sure your codes are valid for the date of service.
Final Word: Get the Code Right, Get Paid Right
The DX code for CHF ICD-10 is not just a billing detail — it is the foundation of your reimbursement strategy for one of the most common cardiac diagnoses in America. In 2026, with payers running tighter audits and CMS putting more pressure on specificity, the coders and practices that win are the ones who take documentation seriously, query when needed, and never settle for I50.9 when the chart tells a more specific story.
Nail your CHF codes, and the revenue will follow. Keep guessing, and the denials will keep coming. The choice — and the power — is yours.