What Is the ICD 10 Code for Low Back Pain in 2026?
If you work in medical billing, physical therapy, orthopedics, or primary care, you already know that back pain claims hit your desk every single day. And right now in 2026, the most important code you need to get right is M54.50 — low back pain, unspecified. This is the official ICD 10 code for low back pain that replaced the old, retired M54.5 code, and using the wrong one still gets claims denied automatically.
So let’s break this all the way down — what the code means, when to use it, when NOT to use it, how to bill chronic cases correctly, and what updates hit the 2026 ICD-10-CM code set that every coder needs to know right now.
Whether you are a coder, provider, biller, or just trying to understand your diagnosis paperwork, this guide covers everything in plain American English.
What Does M54.50 Mean? (The Real Definition)
M54.50 sits inside the ICD-10-CM Chapter 13: Diseases of the Musculoskeletal System, under the M54 Dorsalgia category. Specifically, it falls under the M54.5 parent code (which is itself non-billable, so you can never submit M54.5 alone on a claim).
M54.50 = Low back pain, unspecified
Here is what that actually means in plain language:
- The patient has pain in the lumbar or lumbosacral region
- There is no documented cause or clearly defined mechanism behind the pain
- No structural pathology has been confirmed yet through imaging or clinical workup
- The pain does not involve radiculopathy, sciatica, or nerve root compression
Think of M54.50 as the “we know where it hurts, but we do not yet know exactly why” code. It is 100% valid in the right clinical situation — specifically early in the episode of care when workup is still ongoing, or when thorough evaluation genuinely finds no identifiable cause.
The code covers conditions also referred to as lumbago not otherwise specified (NOS), loin pain, low back pain NOS, and lumbar pain without specific etiology.
This code became effective October 1, 2021, and the current 2026 edition (FY2026) took effect October 1, 2025, remaining active through September 30, 2026 under HIPAA-covered transactions.
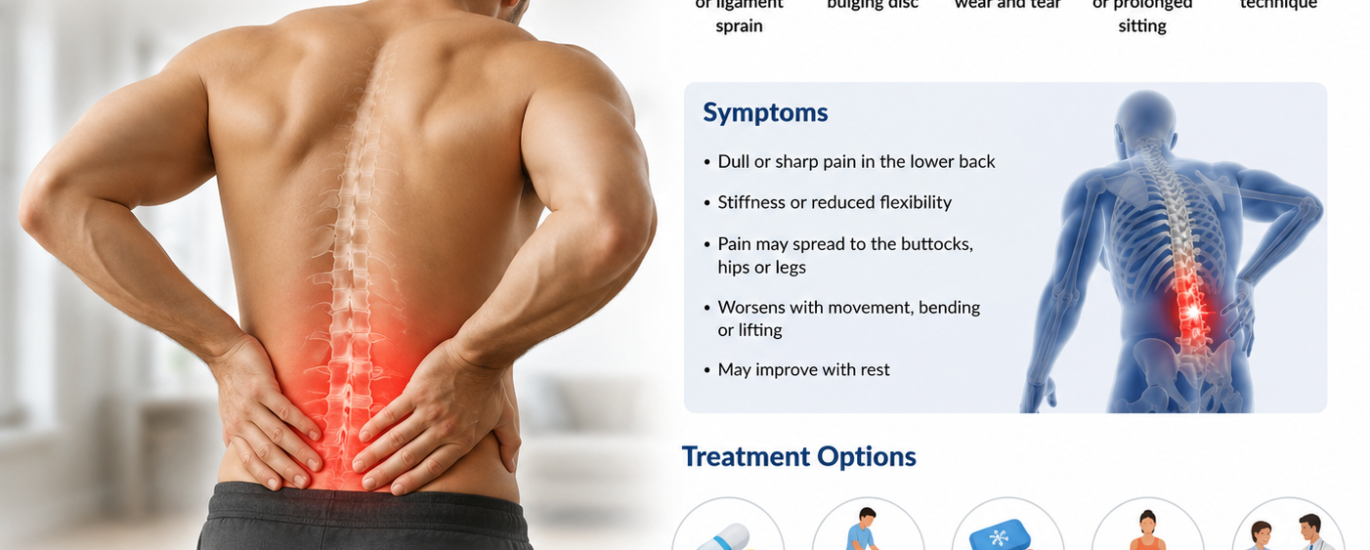
Symptoms Associated with Low Back Pain (M54.50)
Since M54.50 is an unspecified code, the symptoms that push a provider to use it are typically non-specific in nature. That actually helps define when it is appropriate. Here are the most common presentations that correctly map to this icd 10 code for lower back pain:
- Dull, aching pain localized to the lumbar region (lower back)
- Pain that worsens with prolonged sitting, standing, or bending
- Stiffness in the morning that eases with movement
- Muscle tightness or soreness across the low back
- Pain that does NOT radiate down the leg (no sciatica)
- No neurological symptoms like numbness, tingling, or weakness in the legs
When symptoms go beyond these, you likely need a more specific code. For instance, if the patient reports shooting pain down the leg, that clinical picture moves into sciatica territory (M54.30-M54.32) or lumbago with sciatica (M54.41-M54.42), not M54.50.
The key clinical test for M54.50 is this: after the assessment, can the provider clearly name a structural or neurological cause? If yes, a more specific code exists. If no, M54.50 is your answer.
Common Causes of Low Back Pain
Understanding what causes low back pain helps providers document properly, which in turn supports accurate ICD 10 code for low back pain selection. The most frequent causes fall into a few distinct categories.
Musculoskeletal Causes
Muscle or ligament strain from improper lifting or sudden movement is probably the most common driver. Poor posture held over long periods also overloads the lumbar spine significantly. Weak core and hip muscles that cannot stabilize properly put extra stress on lumbar structures, and myofascial pain and trigger points in lumbar musculature round out this category.
Structural Causes
Intervertebral disc degeneration moves the coding to M51.36x or M51.37x once confirmed. Herniated lumbar discs with or without nerve compression, lumbar spinal stenosis, lumbar spondylosis, and vertebral endplate changes (Modic changes, which code to M54.51 when confirmed) all fall here.
Lifestyle and Systemic Factors
Obesity places excess mechanical load on the lumbar spine and accelerates degeneration. Sedentary lifestyle reduces the spinal stabilization muscles need to function correctly. Occupational repetitive stress in jobs involving heavy lifting or prolonged bending creates cumulative damage over time. Psychosocial contributors including anxiety, depression, and chronic high stress also influence how low back pain develops and persists.
Why does this matter for coding? Because once any structural cause gets formally documented by the provider, the code shifts away from M54.50. For example, once imaging confirms disc degeneration as the source, you move to M51.360 or M51.370, and there is a hard Excludes1 relationship between those codes and M54.50 — meaning you cannot bill both on the same claim.
The Full ICD 10 Code for Low Back Pain Family in 2026
This is where a lot of coders get tripped up. The icd 10 code for low back pain is not just one code — there is a whole family under M54.5x, and each member has distinct documentation requirements. Here is how the group breaks down for FY2026:
M54.50 — Low Back Pain, Unspecified
Use when no cause is documented, workup is incomplete, or pain is truly non-specific. Documentation needs to establish lumbar region pain without identified etiology or radicular component.
M54.51 — Vertebrogenic Low Back Pain
Use when the provider documents vertebrogenic features, typically MRI-confirmed Modic Type 1 or Type 2 endplate changes. The clinician’s assessment must explicitly name vertebrogenic or endplate pathology — imaging reports alone do not support this code. This is one of the most audited codes in the M54 family because coders sometimes assign it based on imaging without the physician’s narrative confirming the mechanism.
M54.59 — Other Low Back Pain
Use when pain is clearly described with a mechanism (mechanical, muscular, facet-mediated, sacroiliac region) but that mechanism is neither unspecified nor vertebrogenic. This code works best in physical therapy, rehab, and primary care encounters where the clinical picture is detailed enough to name a source but does not reach vertebrogenic or radicular territory.
The golden rule: Always assign the most specific code the documentation supports. Default to M54.50 only when the documentation genuinely leaves the cause unresolved.
ICD 10 Code for Chronic Low Back Pain — How to Do It Right
Here is where so many billers and coders go wrong. A lot of people search for a single icd 10 code for chronic low back pain expecting to find one dedicated code — but that single code does not exist in ICD-10-CM.
Instead, the right way to code chronic low back pain in 2026 uses a two-code combination:
- Primary Diagnosis: M54.50 (or M54.51 / M54.59 based on documentation)
- Secondary Diagnosis: G89.29 — Other Chronic Pain
That combination together is how you signal to the payer that this is not a brand-new complaint. Without adding G89.29, every single visit looks like an acute presentation, and payers may then deny or limit authorization for treatments like physical therapy, advanced imaging, or pain management interventions that they typically reserve for chronic conditions.
Key documentation rule for chronic coding: Your provider must document pain persisting for 12 weeks or more. That is the threshold that justifies G89.29 on the claim.
Sequencing matters too. If the encounter focuses on evaluating or treating the back condition itself, M54.50 goes first as primary and G89.29 comes second. If the encounter is specifically for chronic pain management — like an injection visit or pain management consult — sequence G89.29 first instead.
Acute on chronic situations happen all the time. Someone with established chronic low back pain tweaks their back doing yard work. In that case, code the acute condition (M54.5x) as primary and attach G89.29 as secondary, with a clear provider note in the chart linking the acute episode to the existing chronic condition.
This is the correct icd 10 code for chronic lower back pain workflow in 2026, and it keeps your claims clean.
2026 ICD-10-CM Updates You Need to Know
The good news for FY2026 is that the M54 Dorsalgia category itself has not undergone major structural changes. M54.50, M54.51, and M54.59 all remain defined exactly as they were under CMS guidelines for this fiscal year (October 1, 2025 through September 30, 2026).
However, several updates from recent cycles remain highly relevant to every low back pain claim in 2026.
Expanded Sixth-Character Detail for Disc Degeneration (M51.36x and M51.37x)
CMS introduced expanded sixth characters for lumbar (M51.36x) and lumbosacral (M51.37x) disc degeneration codes. These differentiate between back pain only (suffix 0), leg pain only (suffix 1), combined back and leg pain (suffix 2), and no specified pain location (suffix 9). This matters enormously because M51.360 carries a direct Excludes1 relationship with M54.50. If disc degeneration with discogenic back pain is confirmed, M54.50 is excluded by rule and cannot appear on the same claim.
Medicare Acupuncture Coverage Monitoring
CMS continues evaluating the chronic low back pain acupuncture National Coverage Determination. Practices billing Medicare acupuncture for low back pain should check their MAC’s Local Coverage Determination at least annually to confirm M54.50 and related codes remain on the covered diagnosis list, since LCD-level updates can affect coverage without any changes to the NCD itself.
The April 1, 2026 Mid-Year Update
The mid-year CMS update effective April 1, 2026 did not introduce new codes within the M54.5x family. Still, practices should review updated payer policies following this cycle — particularly around how payers are treating unspecified diagnosis codes going into the second half of the fiscal year.
MS-DRG v43.0 Grouping
For inpatient claims, M54.50 continues grouping within Diagnostic Related Group assignments under MS-DRG Version 43.0, applicable from October 1, 2025 through September 30, 2026.
Smart Billing Tips for M54.50 Claims in 2026
Getting M54.50 claims paid cleanly comes down to documentation quality and code selection discipline. Here are the most actionable billing tips working coders and billers are using right now.
Tip 1: Document Why the Cause Is Unspecified
Do not just write “low back pain” in the assessment. Instead, have providers note something like: “Low back pain, lumbar region, no radicular symptoms, cause not yet determined pending further workup.” That one sentence justifies M54.50 and reduces payer scrutiny significantly.
Tip 2: Update the Code as the Workup Matures
M54.50 is appropriate early in an episode of care. However, once imaging, physical exam, or specialist evaluation identifies a cause, the code must be updated to match. Keeping M54.50 across multiple visits after findings emerge is one of the top audit triggers payers watch for.
Tip 3: Verify Excludes1 Rules Before Submitting
Before hitting submit on any low back pain claim, check that you are not combining M54.50 with any of its excluded codes. The most important exclusions to remember are low back strain (S39.012), lumbago with sciatica (M54.41 or M54.42), intervertebral disc displacement (M51.2x), and disc degeneration with discogenic pain (M51.360, M51.370).
Tip 4: Pair G89.29 Correctly for Chronic Cases
For any patient with documented pain lasting 12 or more weeks, always add G89.29 as secondary. Never let a chronic patient’s claim go out looking acute — payers use that to deny physical therapy authorizations and pain management services.
Tip 5: Build Payer-Specific Pre-Submission Reviews
Not all payers treat M54.50 the same way. Commercial payers often scrutinize unspecified codes more aggressively than Medicare in primary care settings. Build a pre-submission check into your workflow that flags M54.50 claims without solid supporting documentation before they leave your system.
Tip 6: Watch Your CPT-ICD-10 Pairings
Common CPT pairings with M54.50 include evaluation and management codes, physical therapy procedure codes, and imaging orders for lumbar MRI or X-ray. Always verify medical necessity and payer-specific policies before pairing any CPT with M54.50. An E/M code at the highest complexity level paired with M54.50 and thin documentation is a combination that draws payer attention fast.
Related ICD-10 Codes Every Low Back Pain Coder Should Know
Alongside the icd 10 code for low back pain unspecified, every coder in this space should know these closely related codes cold:
| Code | Description | Key Use |
|---|---|---|
| M54.51 | Vertebrogenic low back pain | Endplate pathology MRI-confirmed |
| M54.59 | Other low back pain | Mechanical or muscular, clearly described |
| M54.16 | Lumbar radiculopathy | Nerve root irritation, lumbar region |
| M54.30-M54.32 | Sciatica | Without coexistent low back pain |
| M54.41, M54.42 | Lumbago with sciatica | LBP WITH sciatic nerve involvement |
| M51.26 | Disc displacement, lumbar | Disc herniation confirmed |
| M51.360 | Lumbar disc degeneration, discogenic back pain | Excludes1 with M54.50 |
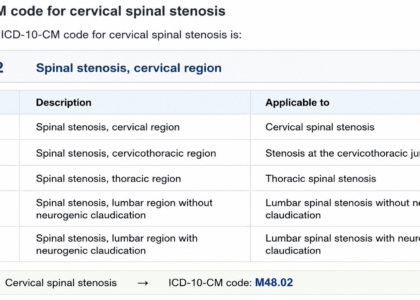
| M48.061-M48.062 | Lumbar spinal stenosis | Canal narrowing confirmed |
| M47.816 | Lumbar spondylosis | Degenerative arthritic changes |
| S39.012 | Low back strain | Traumatic mechanism; Excludes1 with M54.50 |
| G89.29 | Other chronic pain | Secondary code for chronic presentations |
| G89.4 | Chronic pain syndrome | Multifactorial, persistent pain |
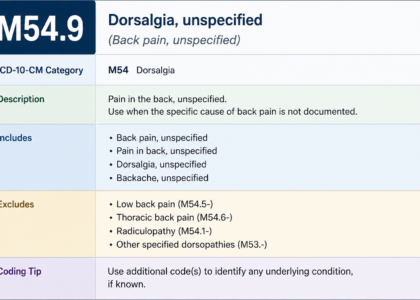
| M54.9 | Dorsalgia, unspecified | General back pain NOS |
Understanding how these codes relate to M54.50 helps you select the right one every time rather than defaulting to the unspecified option out of habit.
Common Mistakes That Get Low Back Pain Claims Denied
These are the most frequent coding mistakes happening in 2026 that are costing practices real money on low back pain claims.
Mistake 1: Still Using the Retired M54.5 Code
M54.5 has been a non-billable parent code since October 1, 2021. Yet EHR favorites lists and old superbills still carry it. Submitting M54.5 triggers automatic rejection. Update every template, dropdown, and superbill in your system right now.
Mistake 2: Using M54.50 When Documentation Supports a More Specific Code
This is the single biggest denial trigger in the M54 family. If the chart says “mechanical low back pain” or if imaging reveals disc degeneration, M54.50 is no longer appropriate. Coders must read the entire clinical note and not just grab the first LBP code they see.
Mistake 3: Pairing M54.50 with Excluded Diagnoses
Combining M54.50 with M54.41 (lumbago with sciatica), M51.360 (discogenic pain), or S39.012 (low back strain) on the same claim violates Excludes1 rules. Payers flag and deny these combinations automatically.
Mistake 4: Using M54.50 for Cervical or Thoracic Pain
M54.50 is specific to the lumbar region. Pain in the thoracic spine codes to M54.6. Pain in the cervical region codes to M54.2x. Using M54.50 for upper or mid-back pain is an anatomical mismatch that creates documentation integrity issues and potential compliance problems.
Mistake 5: Not Updating the Code Across Multiple Visits
Repeating M54.50 on visit four and five after imaging findings have come back raises red flags with payers. High-frequency use of unspecified codes across a single episode of care is one of the top patterns that triggers payer audits.
Mistake 6: Billing G89.29 as a Standalone Primary Code
G89.29 always functions as a secondary code when the cause of the chronic pain is identified. It never stands alone as the primary diagnosis when a site-specific code like M54.50 is available to lead the claim.
Mistake 7: Assigning M54.51 Without Imaging-Confirmed Vertebrogenic Pathology
M54.51 requires the clinician to explicitly document vertebrogenic or endplate pathology in their assessment. Coders cannot infer it from an imaging report alone. The physician’s note must name the vertebrogenic mechanism — otherwise the code is unsupported and audit-vulnerable.
A Note on E-E-A-T: Who This Guide Serves
This guide serves medical coders, billers, revenue cycle managers, clinic administrators, physical therapists, orthopedic surgeons, primary care providers, and patients trying to understand their diagnosis paperwork. The information presented throughout reflects the FY2026 ICD-10-CM code set published by CMS, effective October 1, 2025 through September 30, 2026, and aligns with official guidelines from the ICD-10-CM Official Guidelines for Coding and Reporting. Always verify against the current CMS ICD-10-CM code set and consult your payer’s specific LCD/NCD policies before submitting claims, since payer-level rules can vary even within the same national code set.
Frequently Asked Questions (FAQ)
What is the ICD 10 code for low back pain in 2026?
The correct ICD 10 code for low back pain in 2026 is M54.50, which stands for “low back pain, unspecified.” It replaced the retired non-billable code M54.5 and is valid for HIPAA-covered transactions from October 1, 2025 through September 30, 2026.
Is M54.50 the same as the ICD 10 code for lower back pain?
Yes. M54.50 covers both “low back pain” and “lower back pain” in clinical documentation. Both terms refer to the lumbar region, and M54.50 is the appropriate code as long as no more specific documented cause is present.
What is the ICD 10 code for chronic low back pain?
There is no single standalone ICD 10 code for chronic low back pain. The correct approach in 2026 uses M54.50 (or M54.51/M54.59 based on specificity) as the primary diagnosis, with G89.29 (Other chronic pain) as a secondary code when the provider documents pain lasting 12 or more weeks.
What is the ICD 10 code for chronic lower back pain when the cause is known?
If the cause is known and documented — for example, vertebrogenic endplate pathology — use M54.51 as the primary code with G89.29 as secondary for chronic cases. If the mechanism is mechanical or muscular but clearly described, use M54.59 with G89.29.
Can I still use M54.5 for low back pain in 2026?
No. M54.5 is a non-billable parent code since October 1, 2021. Submitting it results in automatic claim rejection. Always use M54.50, M54.51, or M54.59 depending on what the provider documented.
What is the difference between M54.50 and M54.51?
M54.50 is for low back pain where the cause is unspecified or unknown. M54.51 is specifically for vertebrogenic low back pain, where the pain originates from vertebral endplate pathology confirmed by imaging and explicitly noted in the clinician’s assessment. You cannot use M54.51 based on imaging alone.
When should I use M54.59 instead of M54.50?
Use M54.59 when the provider’s documentation describes a specific mechanism — such as mechanical, muscular, myofascial, or facet-related low back pain — but that description does not rise to vertebrogenic pathology (M54.51). M54.59 sits between fully unspecified (M54.50) and vertebrogenic-specific (M54.51).
Does M54.50 require laterality?
No. M54.50 does not require laterality. Laterality requirements apply to adjacent codes like sciatica (M54.31 right, M54.32 left) and lumbago with sciatica (M54.41 right, M54.42 left), but not to the M54.5x group itself.
Is low back pain a leading cause of disability?
Yes. Low back pain is the single leading cause of disability worldwide. In the United States, nearly four out of ten adults report experiencing back pain within any given three-month window, making it one of the highest-volume diagnoses submitted to payers every day.
What CPT codes pair commonly with M54.50?
Common CPT pairings include office visit E/M codes (99202-99215), physical therapy procedure codes, lumbar imaging orders, and pain management procedures. Always verify medical necessity and payer-specific policies before pairing any CPT with M54.50.
Final Thoughts: Get It Right Every Time
The icd 10 code for low back pain unspecified — M54.50 — is one of the most used and most misused codes in outpatient billing right now. Used correctly, it is completely valid and gets paid without issue. Used as a lazy catch-all or held onto past the point where documentation supports something more specific, it becomes your biggest reimbursement headache.
The bottom line for 2026 is simple: match your code to your documentation, update it as the clinical picture evolves, pair G89.29 when chronic pain is established, and stay current with CMS annual updates every October 1. Do those four things consistently, and your low back pain claims stay clean.
Low back pain is not going anywhere as a diagnosis. Neither is the demand for coders and billers who understand the M54.5x family inside and out. That expertise is worth building, and this guide gives you the foundation to do exactly that.
This article reflects the 2026 ICD-10-CM FY2026 code set, effective October 1, 2025 through September 30, 2026. Always verify codes against current CMS publications before claim submission.
ICD 10 code for low back pain Slug: icd-10-code-for-low-back-pain-m54-50-2026-guide Meta Title: ICD 10 Code for Low Back Pain (M54.50) – 2026 Guide Meta Description: Learn the 2026 ICD 10 code for low back pain (M54.50). Billing tips, common mistakes, related codes & chronic low back pain coding explained.