If you work in medical billing, clinical documentation, or pain management, you have probably come across diagnosis code G89.29 more than once. Maybe a claim got denied. Maybe your provider documented “chronic pain” without enough detail and you are not sure which code to drop. Either way, this guide breaks it all down for you in plain English, covering everything from what the code actually means to the latest 2026 updates, billing pitfalls, and real-world coding scenarios you need to know.
Let’s get into it.
What Is Code G89.29? Understanding the Meaning
So, what is code G89.29? Simply put, diagnosis code G89.29 is the ICD-10-CM code for “Other Chronic Pain.” It lives inside Chapter 6 of the ICD-10-CM manual, which covers diseases of the nervous system (G00–G99), specifically under the G89 category titled “Pain, not elsewhere classified.”
The code signals that a patient experiences chronic pain that does not fit neatly into a more specific ICD-10 bucket. Think of it this way: if a patient has clearly documented cancer pain, you use G89.3. If they have chronic pain syndrome, you use G89.4. But when the chronic pain is real, persistent, and documented but does not match any of those narrower codes, G89.29 steps in as the right call.
How the ICD-10 System Defines Chronic Pain
Chronic pain in the context of this code generally means pain lasting three months or longer, though some clinical and payer guidelines reference the six-month mark. What matters most is that the provider explicitly documents it as chronic. No automatic ICD-10 rule converts a time frame into a code. The physician’s own words in the chart drive the coding decision every single time.
What Is Diagnosis Code G89.29 in Practice?
In practice, G89.29 shows up all the time in pain management clinics, physical therapy documentation, orthopedic notes, and primary care encounters. You will see it paired with site-specific codes for conditions like persistent low back pain, unresolved joint pain, long-standing pelvic pain with no identified underlying cause, and chronic widespread pain that does not rise to the level of a fibromyalgia diagnosis.
The key thing to understand right away: G89.29 almost never appears as the only code on a claim. It works as part of a pair, providing the “chronic” context that another code cannot supply on its own.
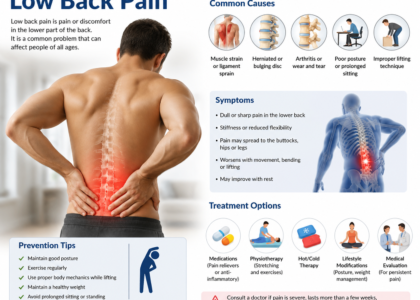
Symptoms Associated with G89.29
Because G89.29 covers “other chronic pain,” the symptoms tied to this code are broad by design. Coders and billers do not diagnose patients, but understanding the clinical picture helps you catch documentation gaps before claims go out the door.
Pain Duration and Functional Impact
Patients coded under G89.29 commonly present with persistent pain lasting beyond three to six months that does not fully resolve with standard treatment. This duration defines the condition. If pain wraps up after a few weeks of anti-inflammatories, it does not qualify here.
Alongside that, pain that interferes with daily activities — including work, sleep, and mobility — is another strong indicator. Providers often document this as functional impairment, and that language carries serious weight when justifying the chronic pain code to payers.
Treatment Resistance and Psychological Overlap
Pain that resists typical acute-phase therapies like rest, NSAIDs, or short-term physical therapy further strengthens the case for G89.29. When patients cycle through multiple interventions without lasting relief, the chronic nature becomes clearer and the documentation path becomes more defensible.
Psychological components — including anxiety, depression, and sleep disturbance — frequently run alongside chronic pain conditions. When a provider documents these connections, coders should consider whether secondary mental health codes are also appropriate alongside G89.29.
When No Clear Cause Exists
No definitive structural or pathological cause identified, or a known cause that cannot fully explain the pain’s severity or persistence, rounds out the clinical picture most commonly associated with G89.29. This scenario shows up most often in primary care and pain management settings.
Importantly, the absence of a clear cause does not mean the pain is not real. G89.29 legitimizes that reality within the billing and documentation system, and providers increasingly rely on it to justify multidisciplinary treatment approaches.
Causes Behind G89.29 Diagnoses
Understanding the causes behind chronic pain coded as G89.29 helps you build more accurate documentation and catch errors during audits. The underlying sources vary widely, which is exactly why this catch-all code exists.
Post-Injury and Degenerative Origins
Post-injury pain that outlives the acute phase ranks as one of the most common drivers. A patient sprains an ankle, heals the structural damage, but continues to experience pain months later. The injury resolves but the pain does not. That lingering experience often lands under G89.29 when no other specific code captures it.
Degenerative conditions like osteoarthritis or degenerative disc disease frequently produce chronic pain that practitioners manage long-term. Even though codes like M54.5x exist for specific back pain sites, the chronic nature of the pain often needs G89.29 as a secondary add-on to tell the full clinical story.
Neuropathic and Inflammatory Drivers
Neuropathic mechanisms play a major role too. When the nervous system becomes sensitized after injury or illness, pain signals keep firing even without ongoing tissue damage. Clinicians call this central sensitization — a recognized clinical phenomenon and a common reason providers document chronic pain without a clear ongoing structural cause.
Inflammatory conditions that practitioners partially treat but never fully resolve also generate G89.29 coding regularly. Systemic conditions like lupus or rheumatoid arthritis in patients who still experience breakthrough pain despite treatment fall into this category. So does chronic pelvic pain in both men and women when imaging and labs rule out gynecological, urological, or gastrointestinal causes.
Is G89.29 a Billable Code?
Yes, absolutely. This question comes up constantly, and the answer is clear. G89.29 is a billable ICD-10-CM code. Payers accept it for reimbursement when coders use it correctly. The 2026 edition of ICD-10-CM confirms its billable status, effective from October 1, 2025, through September 30, 2026.
What Billable Actually Means Here
Being billable means you can submit this code on a HIPAA-covered claim transaction and payers will recognize it. However, “billable” does not mean “always correct” or “always paid.” Payers deny claims when coders sequence the code incorrectly, leave out supporting documentation, or apply it outside the official guidelines.
So yes, G89.29 is a billable code. But using it correctly is what actually gets you paid.
Can G89.29 Be a Primary Diagnosis?
This is where a lot of coders get tripped up, and it is also one of the most searched questions about this code. Yes, G89.29 can be a primary diagnosis, but only in specific circumstances.
When Pain Management Drives the Encounter
According to ICD-10-CM Official Guidelines, a code from the G89 category can lead as the primary or principal diagnosis when the reason for the encounter is pain control or pain management. If a patient comes in specifically to have their chronic pain evaluated and treated as the central purpose of the visit, G89.29 leads the code sequence.
Here is a real-world example: A patient gets a referral to an interventional pain specialist for a facet joint injection. The clinical history shows chronic low back pain from degenerative disc disease. Because the entire purpose of that encounter is pain management — not treating the underlying spinal condition itself — G89.29 goes first as the primary code. The degenerative disc condition code follows as an additional diagnosis.
When Another Condition Takes the Lead
Flip the scenario: A patient visits an orthopedic surgeon to have a herniated disc surgically repaired. Even if chronic pain is a major complaint, the structural condition drives the reason for the encounter. In that case, the disc condition code takes primary position, and coders would typically leave G89.29 off the claim because a definitive diagnosis explains the pain.
One more scenario worth knowing: when a patient presents with pain in a specific location and no definitive diagnosis has emerged, the site-specific pain code goes first, and G89.29 follows as a secondary code to flag the chronic nature.
The bottom line: G89.29 as a primary diagnosis works when pain management explicitly drives the encounter. Otherwise, it rides as a secondary code.
Billing Tips for Diagnosis Code G89.29
Getting G89.29 right on claims means understanding both the coding rules and the payer behavior that surrounds this code. These practical billing tips will save you from denials.
Always Pair G89.29 with a Site-Specific Code
The code tells payers the pain is chronic, but it does not tell them where the pain lives. Payers want both pieces of information. For chronic low back pain, you combine a site-specific M54.5x code with G89.29 to show both the location and the chronic nature. Without that pairing, payers often deny or downgrade claims immediately.
Watch Your Sequencing Carefully
When the visit focuses on pain management, G89.29 goes first. When the visit addresses something else and chronic pain is a documented secondary condition, the primary condition leads. Sequencing errors top the list of reasons G89.29 claims come back denied.
Get Duration Into the Documentation
Coders cannot create chronic status from thin air. The provider must write it in the notes. Language like “patient has experienced pain for over six months with no resolution” or “chronic pain, not responsive to conservative treatment” gives coders the foundation they need to code G89.29 with confidence.
Add Z79.891 for Long-Term Opioid Use
If a patient takes long-term prescribed opioid analgesics as part of their chronic pain management, add Z79.891 as a secondary code. Payers increasingly expect to see this in pain management claims, and leaving it out can raise flags during audits.
Avoid G89.29 When a More Specific Code Exists
If the provider identifies fibromyalgia, use M79.10. If central pain syndrome applies, use G89.0. G89.29 handles the cases that fall through the cracks — not pain that has a clearly coded home in the ICD-10 system.
Keep Documentation Audit-Ready
Medicare and commercial payers have been stepping up scrutiny on chronic pain coding throughout 2025 and into 2026. Your documentation should clearly show duration, functional impact, treatment history, and the provider’s clinical reasoning for why this pain qualifies as chronic. Build that habit now and audits become far less stressful.
Related ICD-10 Codes You Need to Know
Understanding G89.29 also means knowing where it sits in relation to the codes around it. Here is a quick reference every coder in pain management should keep close.
G89.0 – Central Pain Syndrome: This code covers pain disorders that stem from damage to the central nervous system, such as from strokes, spinal cord injuries, or multiple sclerosis. Do not use G89.29 for these cases.
G89.2 – Chronic Pain, Not Elsewhere Classified: This is the parent subcategory that contains G89.29. The full subcategory includes G89.21 for chronic pain due to trauma and G89.28 for other chronic postprocedural pain.
G89.21 – Chronic Pain Due to Trauma: If the chronic pain traces back specifically to a documented traumatic event, this code beats G89.29 for specificity.
G89.28 – Other Chronic Postprocedural Pain: When a patient has lasting pain following surgery or another medical procedure and the pain does not match a more specific code, G89.28 applies rather than G89.29.
G89.3 – Neoplasm-Related Pain: Any chronic pain that a provider associates with cancer, whether primary or metastatic, goes here. G89.29 does not work for cancer pain.
G89.4 – Chronic Pain Syndrome: This code applies when a patient has chronic pain accompanied by significant psychological and social dysfunction. It is not interchangeable with G89.29.
M54.5x – Low Back Pain (site-specific): Frequently paired with G89.29 to build a complete chronic low back pain claim.
M79.10 – Fibromyalgia, Unspecified: Use this instead of G89.29 when the provider confirms fibromyalgia as the diagnosis.
Common Mistakes Coders Make with G89.29
Billing errors around this code show up surprisingly often, even among experienced coders. Knowing the traps helps you avoid them.
Flying Solo Without a Site-Specific Code
Using G89.29 alone without a site-specific code is the most frequent mistake. Payers see an isolated G89.29 and question the claim immediately because no context tells them where the pain lives. Always bring a location-specific partner code along.
Getting Sequencing Backwards
Missequencing the code comes in as a close second. Dropping G89.29 as primary when the visit is a routine follow-up for a known structural condition — rather than a dedicated pain management encounter — leads directly to denials and audit flags.
Ignoring More Specific Options
Coding G89.29 when a more specific code exists undermines claim accuracy. If the pain has a specific ICD-10 home, use that code. Reserve G89.29 for genuinely “other” chronic pain situations where nothing more precise fits.
Assuming Chronicity Without Documentation
Relying on assumed chronicity instead of documented chronicity creates compliance exposure. Just because a patient has come in repeatedly for pain does not mean you can infer the provider considers it chronic. That specific language must appear in the note.
Mixing Up G89.29 and G89.4
Confusing G89.29 with G89.4 trips up many coders. G89.4 requires documentation of the full chronic pain syndrome picture, including psychological and behavioral components. Applying G89.4 when the documentation only supports general chronic pain is a coding error that can invite audit attention.
2026 Updates for Diagnosis Code G89.29
The 2026 ICD-10-CM edition, effective October 1, 2025, keeps G89.29 as a valid and billable code with no changes to its definition or excludes notes. However, several developments in the broader coding environment change how you should handle this code going forward.
MS-DRG v43.0 and Inpatient Grouping
MS-DRG v43.0 grouping is now in effect, and G89.29 falls within updated diagnostic related groups for inpatient claims. If your facility handles inpatient pain management encounters, review the new DRG assignments to confirm that G89.29 contributes correctly to the grouping logic.
Increased Payer Scrutiny in 2026
Payer scrutiny on chronic pain claims is climbing in 2026. Both Medicare Advantage plans and commercial payers have tightened their review of pain management coding, particularly around opioid-related treatment claims. Expect more pre-authorization requirements and documentation reviews for encounters where G89.29 appears.
AI-Assisted Coding Tool Integration
AI-assisted coding tools now run across major health systems, and many of them flag G89.29 as requiring secondary code pairing validation before submission. If your facility runs automated coding software, build a workflow check that confirms site-specific codes always accompany G89.29 before claims go out the door.
Telehealth Documentation Standards
Telehealth pain management visits continue to generate G89.29 questions in 2026. The coding rules have not shifted for virtual encounters, but documentation standards apply equally. Chronic pain that a provider documents during a telehealth visit carries the exact same coding requirements as an in-person one.
Frequently Asked Questions
What is diagnosis code G89.29?
Diagnosis code G89.29 is the ICD-10-CM code for “Other Chronic Pain.” It classifies persistent pain lasting three months or more that does not fall under a more specific chronic pain code. It sits under the G89 category — pain not elsewhere classified — within Chapter 6 of the ICD-10-CM.
Is G89.29 a billable code?
Yes. G89.29 is a fully billable and specific ICD-10-CM code for fiscal year 2026, valid for HIPAA-covered claim submissions from October 1, 2025, through September 30, 2026.
Can G89.29 be a primary diagnosis?
Yes, but only when the specific reason for the patient encounter is pain control or pain management. In most other visit types, G89.29 functions as a secondary code alongside a site-specific diagnosis.
What code is G89.29 grouped under?
G89.29 sits under subcategory G89.2 (Chronic Pain, Not Elsewhere Classified), inside the G89 parent category for Pain, Not Elsewhere Classified. The full hierarchy runs: G00–G99 → G89 → G89.2 → G89.29.
What is the difference between G89.29 and G89.4?
G89.29 covers chronic pain that lacks a more specific ICD-10 designation. G89.4 covers chronic pain syndrome — a condition where long-term pain produces measurable psychological, social, and behavioral dysfunction. Documentation must support the full syndrome picture before you code G89.4.
Can G89.29 pair with M54.5 for chronic back pain?
Yes, and this combination is both common and correct. Use the appropriate M54.5x code as primary to identify the back pain location, then add G89.29 as the secondary code to flag the chronic nature of the condition.
Why did my claim get denied when I used G89.29 as the primary diagnosis?
Most G89.29 primary diagnosis denials happen because the visit was not specifically for pain management, or because the claim was missing the site-specific secondary code. Review the provider’s documentation to confirm the encounter purpose, verify the location-specific code accompanies G89.29, and resubmit with corrected sequencing.
Does G89.29 apply to mental health-related chronic pain?
Not directly. When a provider links chronic pain specifically to a psychiatric condition, the coding path shifts. However, mental health codes can run alongside G89.29 when both conditions receive separate documentation and attention during the same encounter.
Final Takeaway
Diagnosis code G89.29 sounds simple on the surface but carries a lot of nuance underneath. Getting it right means understanding when it leads, when it follows, and when it should not appear at all. Providers need to document the chronic nature of pain in their own words. Coders need to pair the code with location-specific codes every single time. And everyone on the billing team needs to stay current as payer policies tighten throughout 2026.
Whether you are a coder, a biller, a compliance auditor, or a provider who wants to understand the documentation side of things, working with G89.29 effectively comes down to three things: specificity, sequencing, and solid clinical notes. Master those three, and this code stops generating denials and starts accurately telling the patient’s story while getting your facility paid the right way.