Healthcare providers and medical coders face a critical decision every single day when documenting patient conditions: which ICD-10 code tells the complete story of a patient’s nerve pain? The choice between M54.17 and M54.16 might seem like splitting hairs, but this distinction directly impacts billing accuracy, reimbursement rates, and patient care documentation quality.
Since January 2026, these two codes remain essential tools in the musculoskeletal disease coding arsenal. Yet many healthcare professionals still struggle with code selection, leading to claim denials, billing delays, and compliance issues. This comprehensive guide clears up the confusion and equips you with the knowledge to select the right code every single time.
Understanding What M54.16 and M54.17 Actually Mean
M54.16 Meaning: Radiculopathy in the Lumbar Region
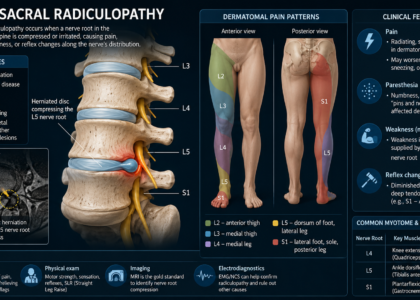
M54.16 specifically addresses nerve root irritation happening in the lumbar spine. This code applies when a patient experiences pain caused by nerve root compression or irritation between the first lumbar vertebra down through the lowest part of the lumbar region, but stops before the sacrum. Think of the lumbar area as your lower back—that’s the sweet spot where M54.16 applies.
The lumbar spine consists of five vertebrae (L1 through L5). When any nerve root in this area gets pinched, inflamed, or irritated, M54.16 becomes your coding choice. This code captures patients who have pure lumbar-level radiculopathy without involvement of the sacral region.
M54.17 Meaning: Radiculopathy in the Lumbosacral Region
M54.17 takes things one step further anatomically. This code applies when nerve root involvement extends into the lumbosacral region—meaning the pain and nerve symptoms involve both the lumbar spine and the sacral region. The sacrum is that triangular bone at the very base of your spine, right above your tailbone.
When a disc herniation, bone spur, or stenosis affects nerve roots in this junction area, M54.17 is your answer. This code essentially says “the problem spans from the lower lumbar area right down into the sacral zone.”
Key Differences: When to Use M54.16 vs M54.17
Anatomical Location Matters Most
The primary distinction between these codes hinges on anatomy. Here’s what separates them:
M54.16 applies when:
- Nerve root compression occurs exclusively in the lumbar region (L1-L5)
- Pain radiates downward but originates from lumbar nerve root irritation
- Imaging confirms the pathology is strictly lumbar
- Documentation specifies lumbar region involvement only
M54.17 applies when:
- Nerve root compression involves the lumbosacral junction
- Symptoms extend into the sacral nerve roots
- The problem spans from lower lumbar vertebrae through the sacral region
- Documentation explicitly mentions lumbosacral involvement
Clinical Presentation Clues
Patients with M54.16 typically report radiating pain down one or both legs originating from the lumbar area. Those with M54.17 often describe similar pain patterns, but the underlying cause involves the sacral transition zone.
Documentation Language Signals Code Selection
Your physician’s documentation is the GPS guiding your code selection. When notes mention “lumbar radiculopathy,” M54.16 fits perfectly. When documentation says “lumbosacral radiculopathy,” M54.17 is the match. It really is that straightforward—code to what the provider documents.
Understanding the Symptoms
Common Radiculopathy Symptoms Across Both Codes
Patients presenting with either M54.16 or M54.17 typically report strikingly similar symptoms. These symptoms include:
Pain Characteristics:
- Sharp, burning, or shooting pain radiating from the lower back down one or both legs
- Numbness and tingling sensations in the buttocks, thighs, calves, or feet
- Weakness in the affected leg or foot affecting normal movement
- Pain that worsens with certain movements like bending forward or lifting heavy objects
- Symptoms that intensify when sitting for extended periods
Neurological Signs:
- Loss of reflexes in the affected leg
- Muscle weakness that impacts walking or performing daily activities
- Loss of sensation in specific dermatomes (nerve distribution patterns)
- Difficulty controlling foot movement or dragging the affected foot
Functional Impact:
- Limited ability to walk distances without stopping
- Difficulty standing upright for extended periods
- Pain during sleep affecting rest quality
- Reduced ability to perform work-related tasks
- Difficulty with stairs or driving
The symptom overlap between M54.16 and M54.17 is why precise anatomical documentation becomes so critical. Both conditions hurt—the difference is where the nerve irritation originates.
Root Causes Behind Both Code Scenarios
What Actually Causes Radiculopathy?
Several underlying conditions create the nerve irritation that these codes describe:
Intervertebral Disc Issues: The most common culprit involves discs slipping, bulging, or herniating out of their normal space. When the soft inner material pushes through the outer ring, it can press directly on nerve roots. This ranks as the leading cause you’ll encounter in your coding practice.
Spinal Stenosis: This degenerative condition narrows the spinal canal or the small openings where nerves exit the spine. As the space shrinks, nerve roots get compressed—particularly common in aging patients.
Spondylosis (Arthritis of the Spine): Bone spurs develop from years of wear and tear. These bony growths can narrow nerve passages and irritate nerve roots over time.
Muscle Tension and Inflammation: Sometimes the piriformis muscle in the buttocks tightens and pinches nearby nerves, creating radicular symptoms. While less common than disc issues, it happens.
Trauma and Injury: Falls, motor vehicle accidents, or sports injuries can cause acute nerve root compression through disc displacement or vertebral misalignment.
Pregnancy and Hormonal Changes: Hormonal shifts loosen ligaments, and increased weight stress the lumbar spine during pregnancy, occasionally triggering radiculopathy.
Poor Posture and Lifestyle Factors: Chronic slouching, heavy lifting, smoking, and being overweight all contribute to developing radiculopathy over time.
Billing and Coding Compliance Tips for 2026
Documentation Requirements You Cannot Ignore
Proper billing starts with bulletproof documentation. Here’s exactly what your medical records must contain to support M54.16 or M54.17 coding:
Essential Documentation Elements:
- Specific anatomical location of nerve involvement (lumbar vs. lumbosacral)
- Clear description of radiating pain pattern and distribution
- Detailed neurological examination findings
- Documentation of numbness, tingling, weakness, or reflexes changes
- Imaging results supporting the diagnosis (MRI, CT, or X-ray findings)
- Laterality information when applicable (right side, left side, or bilateral)
- Physician signature and credentials on all chart entries
- Clear link between documented symptoms and code selection
Why This Matters in 2026: CMS audits have intensified scrutiny on specificity. Vague documentation like “leg pain” triggers denials. Precise documentation like “left lower extremity radicular pain radiating to the lateral foot consistent with L5 nerve root irritation” passes audits every time.
Common Billing Mistakes That Cost Claims
Mistake #1: Using Both Codes Simultaneously Many coders submit both M54.16 and M54.17 on the same claim. This creates conflict signals in the billing system. Use one code based on the anatomical extent of involvement. If documentation is truly unclear, query the provider rather than guessing.
Mistake #2: Overlooking Excludes Notes The ICD-10 manual includes critical “Excludes 1” and “Excludes 2” notations. Never use M54.16 or M54.17 alongside M51.16 (intervertebral disc disorder with radiculopathy, lumbar region) or M51.17 (lumbosacral) on the same claim. These codes already include radiculopathy. If the disc disorder causes the radiculopathy, use the M51 code alone.
Mistake #3: Missing Laterality When Required Some facilities require laterality specification even when the main code doesn’t mandate it. Check your facility’s compliance requirements and your payer’s specific guidelines.
Mistake #4: Failing to Update Codes with New Information If initial documentation suggests M54.16 but subsequent imaging reveals sacral involvement, update to M54.17. Outdated codes don’t reflect current clinical understanding and trigger compliance issues.
Mistake #5: Submitting Without Imaging Support Payers increasingly demand imaging confirmation for radiculopathy diagnosis. MRI results showing disc pathology, stenosis, or nerve root compression significantly strengthen claim defensibility.
Related ICD-10 Codes You Should Know
Understanding the broader coding family helps you select codes precisely:
M54.1 (Radiculopathy, unspecified site): Use only when the exact anatomical location cannot be determined. This non-specific code triggers denials more often.
M51.16 (Intervertebral disc disorder with radiculopathy, lumbar region): Use this instead of M54.16 when a specific disc problem causes the radiculopathy.
M51.17 (Intervertebral disc disorder with radiculopathy, lumbosacral region): The lumbosacral equivalent of M51.16.
M47.26 (Spondylosis with radiculopathy, lumbar region): Use when bone spurs and spinal degeneration cause the nerve irritation.
M54.3 and M54.31-M54.32 (Sciatica codes): Use when pain specifically follows the sciatic nerve distribution.
M54.40-M54.42 (Lumbago with sciatica): Use when both low back pain and sciatic nerve pain are present.
M79.2 (Neuralgia and neuritis): A complementary code sometimes used with radiculopathy codes when inflammation is emphasized.
Understanding these relationships prevents incorrect code submissions and ensures accurate clinical documentation.
Common Coding Mistakes That Medical Professionals Make
The Specificity Trap
Healthcare providers often document “radiculopathy” without specifying whether it’s lumbar or lumbosacral. This forces coders to make assumptions. Instead, coders should query: “Does the patient’s imaging or clinical presentation involve the sacral region, or is this strictly lumbar-level involvement?”
The Disc Disorder Confusion
Many coders use M54.16 when M51.16 would be more accurate and specific. Remember: if documentation clearly links a disc problem to the radiculopathy, the M51 code (disc disorder with radiculopathy) is more specific than M54.16 (radiculopathy without specified cause).
The Bilateral Mishandling
Some coding professionals struggle with bilateral radiculopathy. The base codes M54.16 and M54.17 don’t change for bilateral presentations—they already encompass bilateral cases. However, your documentation must clearly state bilateral involvement so treatment plans and imaging follow-up address both sides.
The Excludes Misinterpretation
Coders sometimes misread “Excludes 1” notes, thinking they can use codes together. They cannot. Excludes 1 means “never use these together.” Check the coding instructions carefully.
The Timing Misalignment
Never code acute radiculopathy the same way as chronic cases developing over months. Documentation should clarify onset timeframe, though the code selection remains the same.
2026 Updates and Current Changes in ICD-10 Coding
What’s New This Year?
Effective Date: The 2026 ICD-10-CM codes became effective October 1, 2025, running through September 30, 2026.
Stability of M54.16 and M54.17: Good news—these codes remain unchanged. No new updates affect their definitions or usage. However, official CMS guidance has sharpened focus on documentation specificity and anatomical precision in 2026.
Enhanced Compliance Focus: CMS has increased post-payment audits specifically targeting radiculopathy coding. They’re examining whether documentation truly supports the code selected. This means:
- Stronger documentation standards become mandatory
- Vague clinical notes trigger automatic denials
- Imaging correlation is increasingly required
- Payer edits have tightened on code combinations
Technology Integration: More practices are implementing AI-powered documentation tools in 2026. These systems flag missing documentation elements before submission, reducing claim rejections.
Telehealth Coding Considerations: As telehealth expands, proper documentation of examination findings and diagnostic considerations becomes even more critical. A virtual visit must document observable neurological signs just as thoroughly as an in-person examination.
Treating and Managing Radiculopathy: A Practical Overview
Conservative Treatment Approaches (First-Line Options)
The vast majority of radiculopathy cases improve without surgery. Conservative management should always be attempted first:
Physical Therapy Benefits: Working with a physical therapist specifically trained in spine care produces remarkable results. Therapy typically focuses on:
- Stretching exercises improving flexibility in the lower back and hamstrings
- Strengthening core muscles supporting the lumbar spine
- Postural correction training improving daily movement patterns
- Manual therapy techniques reducing nerve irritation
- Activity modification strategies preventing symptom aggravation
Most patients experience measurable improvement within 4 to 6 weeks of consistent physical therapy.
Medication Options: Healthcare providers typically recommend medications in this sequence:
- Over-the-Counter NSAIDs: Ibuprofen or naproxen reduce inflammation and provide initial pain relief. These should not continue beyond 10 consecutive days without medical supervision.
- Prescription Neuropathic Agents: Medications like gabapentin and pregabalin specifically target nerve pain. These often work better than traditional NSAIDs for radicular symptoms.
- Muscle Relaxants: Cyclobenzaprine or baclofen ease muscle guarding that worsens nerve compression.
- Oral Corticosteroids: Short courses of prednisone reduce inflammation quickly, providing relief during acute flare-ups.
- Opioid Medications: Reserved for severe pain uncontrolled by other options, these carry addiction risks and should be used cautiously.
Steroid Injections: An epidural steroid injection delivers anti-inflammatory medication directly to the affected nerve root. Guidance from imaging (fluoroscopy or ultrasound) ensures precise placement. Many patients experience 4 to 12 weeks of relief following injection, allowing time for physical therapy to work.
Surgical Intervention: When Conservative Care Fails
Surgery enters the discussion when conservative treatment fails after 12 weeks or when severe neurological deficits threaten permanent nerve damage. Surgical options include:
Lumbar Microdiscectomy: Removes the portion of disc pressing on the nerve root. This is the most common surgical procedure for radiculopathy.
Laminectomy: Removes bone spurs and widens the canal where the nerve root passes, relieving compression from stenosis.
Spinal Fusion: Sometimes performed when instability accompanies radiculopathy, though this more aggressive approach is rarely first-line.
Recovery and Prognosis: What Patients Should Expect
Timeline Expectations
The natural history of radiculopathy shows encouraging patterns:
Weeks 1-4: Most patients notice some improvement with conservative care. Pain intensity often decreases by 30-50% in this window.
Weeks 4-12: Continued improvement occurs with physical therapy compliance. Many patients achieve significant functional recovery by 12 weeks.
3-6 Months: The majority of radiculopathy cases resolve completely with conservative management. Research shows 70-80% of patients experience full resolution without surgery.
Beyond 6 Months: Patients still experiencing symptoms at the six-month mark become candidates for more aggressive interventions like injections or surgery.
Prognosis Factors
Several factors influence recovery speed:
Positive Prognostic Indicators:
- Young age (under 65 years)
- No significant comorbid conditions
- Good physical therapy compliance
- Positive mental health and low stress
- Accurate diagnosis and appropriate treatment
- Strong social and occupational support
Negative Prognostic Indicators:
- Severe baseline neurological deficits
- Chronic pain history
- Smoking status
- Poor physical therapy adherence
- Significant psychological stress
- Litigation or workers’ compensation cases
Frequently Asked Questions About M54.16 and M54.17
Q: Can I use both M54.16 and M54.17 on the same claim?
A: No, absolutely not. These codes address different anatomical regions. Using both together contradicts the diagnosis—the nerve involvement cannot be purely lumbar and also lumbosacral simultaneously. Select the code matching your documentation.
Q: What if documentation says “lumbar region” but the patient has sacral symptoms?
A: Query the provider for clarification. Don’t assume or guess. The provider must specify whether the pathology is lumbar-only or extends into the lumbosacral region. A 30-second query prevents claim denials.
Q: Is M54.16 still appropriate if we find a disc problem on imaging?
A: It depends. If the note says “lumbar radiculopathy, cause unknown,” M54.16 works. However, if imaging clearly shows a disc problem causing the radiculopathy, M51.16 (disc disorder with radiculopathy, lumbar) is more specific and preferred.
Q: How do I handle bilateral radiculopathy in my coding?
A: The base code M54.16 or M54.17 already covers bilateral cases. Your documentation should explicitly state bilateral involvement. Some payers may require modifier RT (right), LT (left), or custom bilateral indicators—check your specific payer requirements.
Q: Do these codes require seventh character extensions?
A: No, M54.16 and M54.17 are complete billable codes without seventh character extensions. Some related codes like spondylosis might require them, but these radiculopathy codes do not.
Q: What’s the 2026 reimbursement rate for M54.16 and M54.17?
A: Reimbursement varies by payer, geographic location, and facility type. Medicare rates differ from commercial insurance. Contact your specific payers for current rates, as these are published annually and may fluctuate.
Q: Can I change from M54.16 to M54.17 during ongoing care?
A: Yes, if new clinical information emerges indicating sacral involvement, updating the code is appropriate. Each visit or encounter receives its own code based on current documentation. However, avoid frequent changes without clear clinical justification, as this triggers audit questions.
Q: What documentation length satisfies compliance auditors?
A: Quality beats quantity. A thorough two-paragraph note clearly describing anatomy, symptoms, examination findings, and imaging correlation outperforms a lengthy vague narrative. Focus on specificity and clarity.
Key Takeaways for Healthcare Professionals
- Anatomy is destiny in code selection—lumbar only means M54.16; lumbar extending into sacral means M54.17.
- Documentation precision directly impacts billing success and compliance. Vague notes trigger denials; specific notes pass audits.
- Never use these codes alongside M51.16/M51.17 or other “definitive diagnosis” codes that already include radiculopathy in their definition.
- Conservative management resolves most radiculopathy cases within 3-6 months without surgical intervention.
- Query when uncertain rather than submitting claims based on assumptions. A 30-second clarification prevents major billing problems.
- Stay current with your specific payer’s coverage policies and documentation requirements—these vary by insurance company.
- 2026 brings increased scrutiny on radiculopathy coding, so documentation standards must be exceptionally tight this year.
Conclusion
The distinction between M54.17 and M54.16 might appear subtle to those outside the medical coding profession, but these four digits represent the difference between appropriate reimbursement and claim denial. Healthcare professionals who master this distinction streamline billing processes, enhance compliance, and ultimately provide better patient care through accurate documentation.
As 2026 unfolds, the CMS emphasis on specificity and documentation accuracy means getting these codes right matters more than ever. Use this guide as your reference when coding encounters radiculopathy, and you’ll navigate this critical area with confidence and accuracy. Remember: when in doubt, query your provider for clarification. That single step prevents cascading billing and compliance problems down the line.