Why Getting These Two Codes Right Matters in 2026
If you work in medical billing, coding, or clinical documentation, you already know that picking the wrong ICD-10 code can mean a denied claim, a payer audit, or delayed reimbursement. And when it comes to neck pain, two codes trip up even experienced coders all the time: M54.2 vs M54.12.
These codes look similar. They both live in the M54 Dorsalgia family. They both deal with the cervical spine. But they are not the same condition, and treating them as interchangeable is one of the most common billing mistakes in outpatient practice today.
So in this guide, we are breaking down everything you need to know about M54.2 vs M54.12 — what each code actually means, what symptoms back each one up, how to document them correctly, and whether you can you bill M54.2 and M54.12 together on the same claim. This guide reflects the 2026 ICD-10-CM edition, effective October 1, 2025.
Let’s get into it.
What Does M54.2 Mean?
M54.2 is the ICD-10-CM code for Cervicalgia — which is simply the clinical word for neck pain. Specifically, it describes pain localized to the cervical spine that does not connect to a more specific structural cause like a herniated disc, a fracture, or confirmed nerve root compression.
The cervical spine runs from the base of your skull down to the upper chest and includes seven vertebrae labeled C1 through C7. When a patient reports pain in that region without clear evidence of nerve involvement or a disc disorder, M54.2 is the code that fits.
Here is the key phrase coders need to keep front of mind: localized, non-radiating neck pain. If the pain stays in the neck and does not travel down the arm, shoulder, or fingers, M54.2 is your code.
According to the 2026 ICD-10-CM guidelines, M54.2 became effective on October 1, 2025, and it covers HIPAA-compliant transactions through September 30, 2026. It is one of the most frequently submitted musculoskeletal diagnosis codes in the United States, appearing on well over 12 million medical claims every single year.
Common Settings Where M54.2 Gets Billed
M54.2 works across a wide range of practice types. Primary care providers use it for initial evaluations. Orthopedic specialists apply it to chronic or injury-related cervical pain. Chiropractors, physical therapists, neurologists, and pain management specialists all bill this code regularly when the documentation supports simple, localized neck pain without radicular features.
What Does M54.12 Mean?
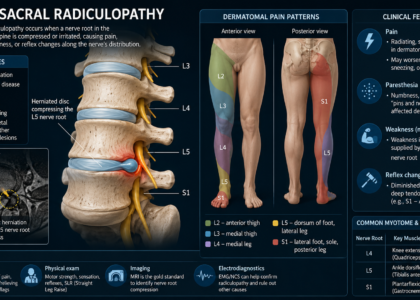
M54.12 is the ICD-10-CM code for Radiculopathy, Cervical Region — sometimes called cervical radiculopathy or cervical radiculitis. This code tells a very different clinical story than M54.2.
Let us break the code down piece by piece:
- M = Disease of the Musculoskeletal System and Connective Tissue
- 54 = Dorsalgia (includes the cervical spine)
- .1 = Radiculopathy (a nerve root is compressed or irritated)
- 2 = Cervical region (the neck)
So M54.12 literally means: musculoskeletal disease involving nerve root compression in the cervical spine. When something presses on a nerve root in the neck — whether from a bone spur, foraminal narrowing, or degenerative changes — that is cervical radiculopathy.
The defining feature of M54.12 is that the pain radiates. It does not just sit in the neck. It shoots down into the shoulder, arm, hand, or fingers. Patients often describe numbness, tingling, burning, or weakness along a specific nerve root pattern.
M54.12 is used in primary care, orthopedics, and neurology. It is a clinically important code because it justifies higher-level services — like nerve conduction studies, advanced imaging, and epidural steroid injections — that would not necessarily be medically necessary for simple cervicalgia.
Symptoms: How to Tell Them Apart Clinically
Getting the diagnosis right starts with understanding what each condition actually looks like in the exam room.
Symptoms of Cervicalgia (M54.2)
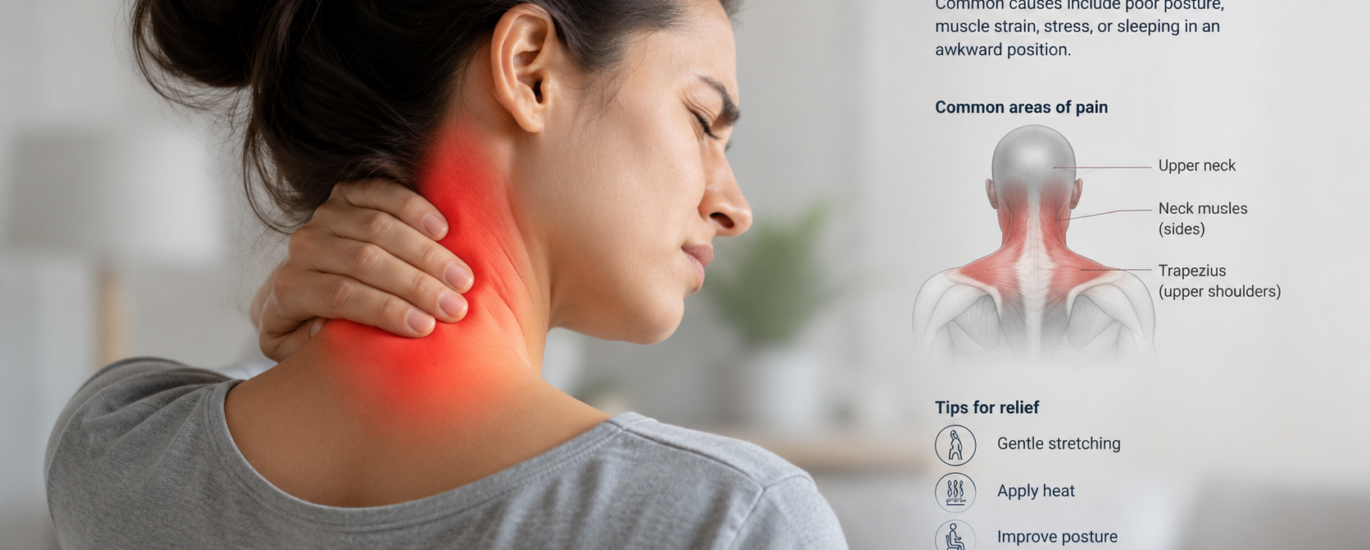
Patients presenting with cervicalgia typically describe pain that is confined to the neck itself. Common symptoms include a dull, aching sensation in the back or sides of the neck, stiffness or tightness that limits head rotation, muscle spasms in the neck and upper shoulders, tenderness on palpation of the cervical muscles, and a sharp or burning sensation with certain movements. Importantly, there are no radiating symptoms — the pain does not travel down the arm or into the fingers.
Symptoms of Cervical Radiculopathy (M54.12)
Cervical radiculopathy presents with a distinctly different picture. The patient reports pain that radiates from the neck into the shoulder and down the arm, sometimes reaching the hand or specific fingers. They may also describe numbness or tingling along a nerve root distribution, muscle weakness in the arm or hand, diminished deep tendon reflexes (like a reduced biceps reflex), and a positive Spurling’s test — where neck extension and lateral rotation reproduce the radiating pain.
That Spurling’s test finding is a big deal. A positive result on physical exam, combined with documented radiating symptoms and imaging correlation, gives you the clinical foundation to support M54.12 on any payer review.
Causes
Causes of M54.2 (Cervicalgia)
Cervicalgia is most often mechanical or postural in nature. Common causes include poor posture from prolonged screen time or desk work, acute muscle strain from sudden movements, minor whiplash without neurological involvement, stress-related muscle tension, and degenerative changes in the cervical spine that produce localized pain but no nerve compression. Sleep position and repetitive occupational movements are also frequent contributors.
Causes of M54.12 (Cervical Radiculopathy)
Cervical radiculopathy results from actual compression or irritation of a nerve root. The most common causes include foraminal stenosis from bone spurs or osteophytes, degenerative disc disease where disc height loss narrows the neural foramen, herniated cervical discs compressing a nerve root at a specific level, and age-related changes where the discs lose hydration and the foramen naturally narrows over time. M54.12 is a non-traumatic code — if the radiculopathy results from an acute injury like a car crash or fall, the provider should use an injury code from the S series instead.
The Difference Between M54.2 and M54.12: A Side-by-Side Breakdown
Understanding the difference between M54.2 and M54.12 is honestly the most important thing you can take away from this entire guide. Here it is in plain language:
| Feature | M54.2 (Cervicalgia) | M54.12 (Cervical Radiculopathy) |
|---|---|---|
| Pain location | Localized to neck | Radiates to arm, hand, or fingers |
| Nerve involvement | None | Nerve root compression confirmed |
| Neurological deficits | Absent | May include weakness, numbness |
| Spurling’s test | Typically negative | Often positive |
| Imaging requirement | Not always needed | MRI or CT often indicated |
| Typical cause | Muscular, postural | Disc, bone spur, foraminal stenosis |
| Code type | Specific, billable | Specific, billable |
The clinical rule of thumb is simple: if pain stays in the neck, use M54.2. If pain travels down the arm, use M54.12.
Misclassifying radiculopathy under M54.2 is actually a common denial trigger, because high-cost services like MRI or epidural injections may not align with a simple cervicalgia diagnosis in severity reviews.
Billing Tips: How to Code M54.2 and M54.12 Correctly in 2026
This is where a lot of practices leave money on the table — or worse, invite audits. Follow these billing tips carefully.
Tip 1: Document to the Level of the Code
For M54.2, your documentation needs to clearly describe localized neck pain without any radiating features, neurological deficits, or confirmed structural cause. Include symptom duration, location, aggravating and relieving factors, and functional limitations. Vague phrases like “neck discomfort” will not hold up if a payer asks for medical necessity.
For M54.12, documentation needs to tell a clear radiculopathy story. That means: the location (cervical), the side (left or right), physical exam findings (Spurling’s test result, reflex changes, sensory changes), and the suspected nerve level (such as C6 or C7). A note like “neck pain radiating to the left thumb and index finger, positive Spurling’s left, reduced left biceps reflex, likely C6 radiculopathy” is the kind of documentation that survives an audit. Without these three elements — location, side, and exam findings — an auditor may downgrade the code to M54.2, which typically reimburses at a lower rate.
Tip 2: Know the Excludes1 Rules
M54.2 carries an important Excludes1 restriction. It cannot be used together with cervical disc disorder codes from the M50 series (like M50.12, which is cervical disc disorder with radiculopathy). These codes are mutually exclusive, meaning they should never appear on the same claim. Doing so will result in a denial.
Similarly, M54.12 cannot be billed alongside M50.12 on the same claim. The disc disorder code is more specific and already includes the radiculopathy component — billing both is effectively double reporting and payers will deny one of them.
Tip 3: Pair Chronic Pain Correctly
If the patient’s cervicalgia or radiculopathy is chronic in nature, add G89.29 (Other Chronic Pain) as a secondary code. This signals to the payer that the condition is not a new, acute complaint and supports authorization for ongoing physical therapy or repeated visits. However, your provider must document that pain has persisted for 12 weeks or more. Vague chart language about “longstanding pain” will not satisfy an auditor looking for a specific timeframe.
Tip 4: Use the Right CPT Pairings
When billing M54.2, appropriate CPT codes include office visits, imaging (X-rays or MRI), physical therapy evaluation and treatment, chiropractic adjustments, and pain management services. When billing M54.12, you can also support CPT codes for nerve conduction studies, electromyography (EMG), and epidural steroid injections, as long as documentation supports medical necessity.
Add Modifier -25 when a significant evaluation and management service is performed on the same day as another procedure. Use Modifier -59 when distinct procedural services are rendered on the same date.
Tip 5: Telehealth Claims Need the Same Documentation Standard
In 2026, telehealth continues to be a major care delivery channel, especially for patients in rural areas. The documentation requirements for M54.2 and M54.12 on telehealth claims are identical to in-person visits. Coders billing these codes on telehealth encounters should confirm payer-specific rules and pair the diagnosis with the appropriate place-of-service code, since Medicare and commercial payers continue to update their telehealth guidance.
Can You Bill M54.2 and M54.12 Together?
This is one of the most searched questions in cervical coding, so let us answer it directly.
Yes — you can bill M54.2 and M54.12 together on the same claim, provided the clinical documentation supports both diagnoses as distinct, co-existing conditions.
Neither M54.2 nor M54.12 lists the other under an Excludes1 note. That means there is no ICD-10-CM rule prohibiting them from appearing together on a claim. When a patient has both localized cervical pain (cervicalgia) and documented nerve root involvement with radiating symptoms (radiculopathy), it is clinically appropriate and coding-compliant to report both codes.
However — and this matters — the documentation must clearly support each diagnosis independently. If the chart simply says “neck pain with arm pain,” that is not enough. The provider needs to document the localized cervical pain separately from the radicular symptoms, with distinct clinical findings for each. Coders should always verify payer-specific policies as well, since some commercial carriers may have their own claim-editing rules that differ from the ICD-10-CM guidelines.
Related ICD-10 Codes to Know
Working with M54.2 and M54.12 effectively also means knowing when a different code is actually more appropriate.
M50.12 — Cervical disc disorder with radiculopathy. Use this instead of M54.12 when a disc disorder is the confirmed cause of the radiculopathy. This code is more specific and should take priority.
M47.812 — Cervical spondylosis without myelopathy or radiculopathy. Use this when degenerative arthritis of the cervical spine is the primary finding, without confirmed nerve root compression.
M48.02 — Spinal stenosis, cervical region. Use this when the cause of neck pain or radicular symptoms is narrowing of the spinal canal.
S13.4XXA — Whiplash injury of cervical spine, initial encounter. Use this for acute traumatic injuries rather than M54.2 or M54.12.
G89.29 — Other chronic pain. Use this as a secondary code with M54.2 or M54.12 when chronicity (12-plus weeks of pain) needs to be flagged.
Common Mistakes That Coders Make With M54.2 and M54.12
Even experienced billing teams make errors with these codes. Here are the most frequent pitfalls to avoid.
Upcoding to M54.12 without documented nerve involvement. If the chart says “neck pain with some arm stiffness” but does not document a positive Spurling’s test, reflex changes, or sensory deficit, you do not have enough support for M54.12. Stick with M54.2 until the documentation catches up.
Using M54.12 for trauma-related radiculopathy. M54.12 is specifically for non-traumatic cervical radiculopathy. If the patient’s nerve root injury resulted from a car accident or fall, the appropriate code comes from the S14 series.
Pairing M54.2 or M54.12 with M50-series disc codes on the same claim. This violates the Excludes1 rule. When a disc disorder is the confirmed cause, the M50 code replaces the M54 code, not supplements it.
Failing to document laterality for M54.12. The code itself does not have built-in left/right specificity. Some payers require documentation of the affected side. Always note in the chart whether symptoms are right-sided, left-sided, or bilateral, and verify your payer’s laterality requirements.
Relying on symptom descriptions alone for M54.12. Radiating pain alone is not always enough. Auditors want to see objective exam findings — reflex changes, dermatomal sensory loss, or weakness — to support a radiculopathy diagnosis.
Submitting M54.2 repeatedly without documentation of improvement or a treatment plan. Some carriers flag repeated M54.2 claims without evidence of a documented plan or functional progress. Always note the treatment approach and any response to prior care.
2026 Updates: What Changed and What to Watch
The 2026 edition of ICD-10-CM became effective on October 1, 2025. Here is what matters for coders working with M54.2 and M54.12 this year.
Both M54.2 and M54.12 remain valid, billable codes in the 2026 edition with no changes to their descriptions or hierarchy. However, the broader M54 code family has seen documentation standards tighten across payers, particularly for claims involving advanced services.
Payer documentation bar continues to rise in 2026. Commercial insurers and Medicare Advantage plans are increasingly requiring functional limitation documentation, treatment plan details, and evidence of care escalation before approving physical therapy extensions or advanced imaging. Coders need to communicate these requirements back to clinical teams proactively.
Telehealth policy remains active. CMS and commercial payers continue to update their telehealth coverage rules, and claims for cervicalgia and radiculopathy via telehealth must meet the same documentation standards as in-person visits.
AI-assisted documentation tools are becoming more common in clinical settings. While these tools can help speed up note generation, coders should review AI-generated notes carefully for specificity — particularly for M54.12, where objective exam findings must be explicitly stated, not inferred.
For acupuncture claims involving chronic neck pain, always verify payer-specific NCD or LCD coverage rules, since not all payers cover acupuncture for cervicalgia the same way they do for low back pain.
FAQ: M54.2 vs M54.12
What is the main difference between M54.2 and M54.12? M54.2 is for localized neck pain (cervicalgia) without nerve involvement. M54.12 is for cervical radiculopathy, where a nerve root in the neck is compressed and pain radiates down the arm. The key distinction is whether pain stays in the neck or travels.
Can you bill M54.2 and M54.12 together? Yes. There is nothing in the ICD-10-CM Excludes1 notes that prohibits billing M54.2 and M54.12 on the same claim. Both can appear together when the documentation supports each diagnosis independently. Always verify individual payer policies.
Is M54.12 a billable ICD-10 code in 2026? Yes. M54.12 is a specific, billable ICD-10-CM code for the 2026 edition, effective October 1, 2025 through September 30, 2026.
When should I use M54.12 instead of M50.12? Use M54.12 when cervical radiculopathy is present but no specific disc disorder has been confirmed as the cause. Use M50.12 when the radiculopathy clearly results from a cervical disc disorder — the disc code is more specific and replaces M54.12 in that scenario.
Can M54.2 be used for chronic neck pain? Yes. M54.2 works for chronic cervicalgia as long as the pain remains localized and non-radiating. Add G89.29 as a secondary code to indicate chronicity, and document that pain has persisted for at least 12 weeks.
Does M54.12 require imaging to support the diagnosis? Imaging is not always strictly required for physician billing, but it significantly strengthens the claim. An MRI or CT showing foraminal stenosis, disc herniation, or bone spur formation at the correlated level gives coders and auditors the objective evidence they need. Without imaging, the physical exam findings need to be especially thorough and clearly documented.
What happens if I use M54.2 when M54.12 is the right code? You risk undercoding. Cervicalgia and radiculopathy have different reimbursement implications. More importantly, using M54.2 when radiculopathy is present can result in denials for associated services — like MRI, nerve studies, or injections — that the payer deems inconsistent with a simple cervicalgia diagnosis in severity.
Final Thoughts: Code Smart, Document Tight
The bottom line on M54.2 vs M54.12 is actually pretty straightforward once you internalize the clinical distinction. M54.2 describes neck pain that stays in the neck. M54.12 describes neck pain that involves a compressed nerve root and radiates out of the neck. They are two different clinical conditions, and they deserve two different codes.
Both are valid, billable ICD-10-CM codes in 2026. Both can appear on the same claim when the documentation supports it. And both require specific, thorough clinical documentation to survive payer scrutiny in today’s environment.
The difference between M54.2 and M54.12 is not just a billing technicality — it tells a patient’s complete clinical story. Code the story right, document the findings specifically, and your claims will process faster, your audits will go smoother, and your revenue cycle will stay healthy all year long.
This article reflects the 2026 ICD-10-CM guidelines effective October 1, 2025. Coding guidance is intended for educational purposes. Always verify payer-specific policies and consult your compliance team for complex billing scenarios.