What Is M54.59 and Why Should You Actually Care?
If you have ever seen the code M54.59 on a medical claim, an explanation of benefits, or a patient’s chart and felt a little lost — you are in good company. This code shows up constantly in physical therapy offices, primary care clinics, chiropractic practices, and pain management centers across the United States. Yet it remains one of the most misunderstood and misapplied codes in the entire M54 family.
So let’s just cut straight to it.
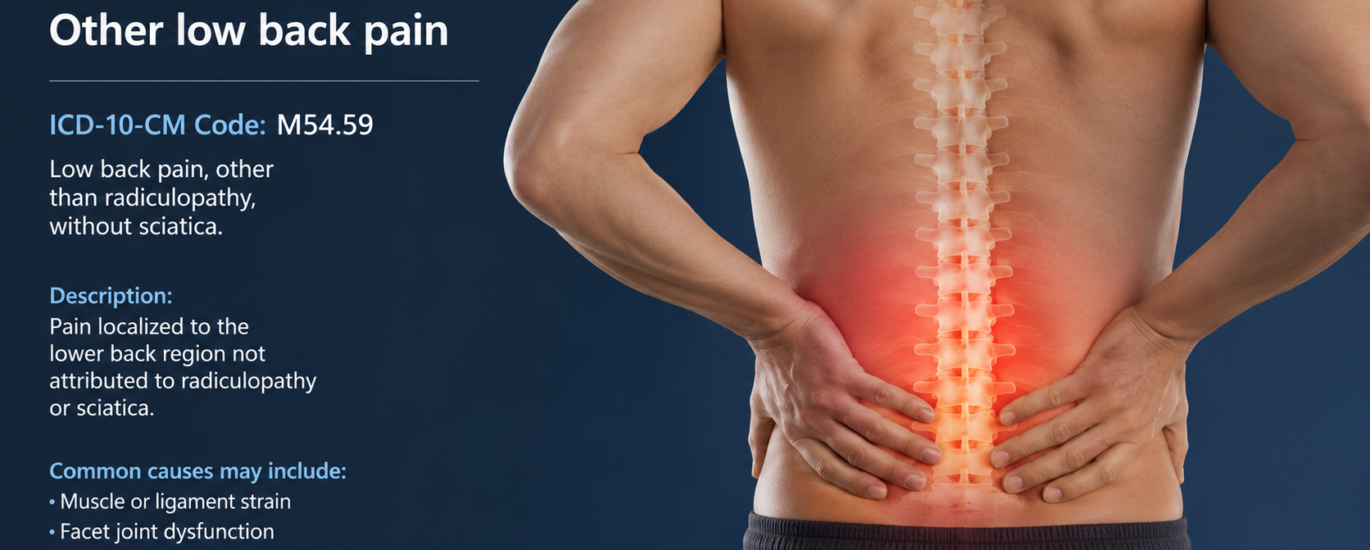
M54.59 is the ICD-10-CM diagnosis code for “Other low back pain.” The 2026 edition of ICD-10-CM confirms this code became effective on October 1, 2025, and remains fully valid and billable through September 30, 2026. That means every claim you submit right now in 2026 for a qualifying low back pain presentation — one that is characterized but does not fit the vertebrogenic category — should carry M54.59, not a vague or incorrect substitute.
This code lives in the M50–M54 dorsopathies chapter, which is the ICD-10-CM section covering diseases of the musculoskeletal system that affect the spine. Specifically, M54.59 sits alongside its two siblings in the M54.5x subcategory:
- M54.50 — Low back pain, unspecified
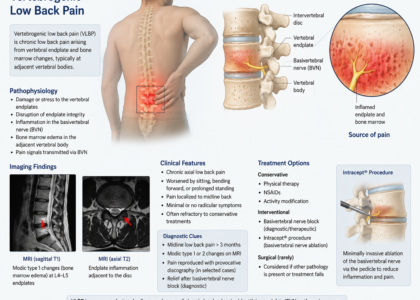
- M54.51 — Vertebrogenic low back pain
- M54.59 — Other low back pain (that’s the one we’re talking about today)
Understanding where M54.59 fits — and more importantly, when to use it versus its siblings — is the difference between clean, first-pass claims and a cascade of denials, audits, and resubmissions.
The History Behind M54.59: Where Did This Code Come From?
Before October 1, 2021, providers and coders across the country were using a single, broad code called M54.5 to describe any and all forms of low back pain. That one code covered everything from a pulled muscle to complex chronic lumbar pain syndromes. CMS and the National Center for Health Statistics finally said enough is enough.
On October 1, 2021, CMS formally retired M54.5 as a billable code and converted it into a non-billable parent code. In its place, three specific child codes went live: M54.50, M54.51, and M54.59. The goal was simple — force greater clinical precision and better data capture across the healthcare system.
M54.59 specifically fills a very important middle ground. It covers all low back pain presentations where the provider has clearly identified a source or mechanism for the pain, but that source is not vertebrogenic (which belongs to M54.51) and the condition does not map cleanly to any other more specific ICD-10 code.
If you or your team is still submitting claims with M54.5 — the version without a fifth digit — those claims are getting auto-rejected. That code has been dead for over four years. No exceptions.
What Does M54.59 Actually Mean Clinically?
This is the part that trips up a lot of coders and even some clinicians. The phrase “other low back pain” sounds like a catch-all, like a trash can for everything that doesn’t fit elsewhere. But that reading is completely wrong.
According to WHO’s ICD-10 classification framework, “Other” subcodes are clinically meaningful categories, not vague leftovers. M54.59 applies specifically when:
- The provider has documented a recognizable, specific pain pattern or mechanism
- That mechanism is not vertebrogenic (not tied to vertebral endplate pathology or Modic changes)
- No other more precise ICD-10-CM subcode exists for that particular presentation
Think of M54.59 as the code for “I know what’s causing this back pain, I can describe it clearly, it just isn’t vertebrogenic and there isn’t a tighter code for it.”
Common clinical scenarios where M54.59 fits perfectly include:
Myofascial low back pain — Pain from muscular trigger points in the paraspinal muscles, with documented tenderness on palpation and reproducible referred pain patterns. The synonym list for M54.59 actually includes myofascial pain specifically.
Mechanical low back pain — Pain that clearly worsens with certain movements, postures, or loading patterns, such as extension-based aggravation or pain that improves with position change. The provider documents the mechanism, but it is not vertebrogenic.
Facet-mediated pain (without a more specific code) — Sometimes facet joint pain does not meet the specificity threshold for M47.8x (spondylosis) codes, yet the clinical exam clearly points to a facet-related source. In those cases, M54.59 steps in.
Soft-tissue injury with a named mechanism — For instance, a patient with a work-related posture injury that has caused chronic paraspinal muscle strain, where the provider names the mechanism clearly but where the injury code family does not cleanly apply.
The critical distinction here: M54.59 is not for pain without a documented cause. That is M54.50. M54.59 demands that the provider actually characterize what is going on. Documentation quality is everything with this code.
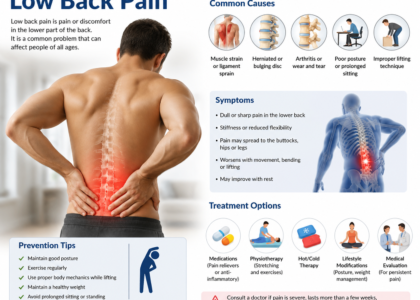
Symptoms Associated with M54.59 Other Low Back Pain
Because M54.59 covers several different clinical presentations of other low back pain, the symptom picture can vary. However, certain patterns show up repeatedly in the types of cases this code captures:
Aching, diffuse lumbar pain that may shift around the lower back rather than staying in one fixed spot. This is common in myofascial presentations where multiple trigger points are involved.
Pain that changes with movement or posture. Mechanical patterns often show clear aggravating and relieving factors. The pain gets worse when sitting for a long time, then improves with walking. Or it flares with repeated bending but eases with lying flat. This kind of documented pattern strongly supports M54.59 over M54.50.
Localized muscle tenderness and stiffness. Patients often report tightness and point tenderness in the paraspinal muscles alongside the spine, which is a classic myofascial feature.
Morning stiffness that loosens up after a few minutes of movement, which is common in facet-related and mechanical presentations.
No significant radiating leg pain. Just like with M54.51, M54.59 describes axial low back pain. Once sciatic nerve involvement or dermatomal leg pain enters the picture, you are looking at different codes entirely, such as M54.4x for lumbago with sciatica.
Pain without neurological deficits. There is no numbness, tingling, or weakness in the legs associated with M54.59 presentations. The moment those symptoms appear, the diagnostic picture shifts toward radiculopathy codes.
What Causes Other Low Back Pain (M54.59)?
Understanding the root causes behind M54.59 presentations helps clinicians document accurately and helps coders make the right call. Here are the most common drivers:
Myofascial Trigger Points
Tight, hyperirritable spots within the paraspinal muscles can generate constant low-grade pain and referred pain patterns. This is one of the most common causes of other low back pain. Prolonged sitting, repetitive lifting, poor ergonomics, and stress all contribute to trigger point formation over time.
Mechanical Dysfunction
Abnormal movement patterns in the lumbar spine — often related to joint hypomobility, muscle imbalances, or postural dysfunction — create mechanical stress that the body eventually reads as pain. Physical therapists identify these patterns constantly through movement assessments, and when they document them clearly, M54.59 is exactly the right code.
Facet Joint Irritation Without Structural Degeneration
The small facet joints at the back of the spine can become irritated and painful without showing full-blown spondylosis on imaging. When a provider documents facet-mediated pain based on clinical findings but the imaging does not rise to the level of a more specific structural code, M54.59 covers the encounter.
Occupational and Postural Strain
Repetitive loading from work activities — whether it is long hours at a desk, repeated bending and lifting, or prolonged standing — causes cumulative soft-tissue stress that eventually produces a documented pain pattern. When providers name the occupational mechanism, M54.59 fits better than M54.50.
Obesity and Metabolic Factors
Excess body weight significantly increases the mechanical load on the lumbar spine. Over time, this contributes to soft-tissue fatigue and chronic paraspinal muscle pain. When obesity is listed as a contributing factor alongside a documented pain mechanism, coding it as other low back pain with a secondary obesity code provides a complete clinical picture.
Aging and Degenerative Soft-Tissue Changes
As the body ages, the paraspinal muscles, ligaments, and connective tissues around the spine naturally lose elasticity and resilience. This makes the lumbar region more susceptible to strain and slower to recover — often producing the type of generalized but characterizable pain that M54.59 captures.
M54.59 vs M54.50: The Difference That Actually Matters
This comparison comes up constantly in coding departments, and it is worth getting crystal clear on it.
Think of it this way. M54.50 simply means the patient has low back pain, but the details are unclear. The cause has not been identified, the source is not documented, and there is no defined pain pattern. It represents unspecified low back pain.
M54.59 says: “The patient has low back pain, and here is specifically what kind it is — even if it does not fit neatly into the vertebrogenic box.” The provider has done their job and characterized the pain.
The difference comes down entirely to what the clinician documented. If the note says nothing more than “low back pain” or “lumbago,” that is M54.50. If the note says “mechanical low back pain with extension-based aggravation” or “myofascial low back pain with paraspinal trigger points,” that is M54.59.
Practically speaking, M54.59 often requires better documentation and earns greater respect from payers — because it shows that the provider actually assessed the patient and identified a clinical pattern rather than just writing down a generic complaint.
Billing Tips for M54.59 in 2026
Getting the billing right with M54.59 is not rocket science, but it does require attention to detail. Here are the most important tips for coders and billing teams working with this code in 2026:
Nail the Documentation First
M54.59 lives and dies by provider documentation. The note must describe a specific pain source or mechanism. Encourage providers to use language like “mechanical low back pain,” “myofascial pain syndrome,” “facet-mediated lumbar pain,” or “paraspinal trigger point pain” rather than just “low back pain.” Without that specificity in the chart, you default to M54.50 — and that is a step backward clinically.
Do Not Pair M54.59 with Codes That Already Explain the Pain
This is the most common billing mistake with this code. You cannot submit M54.59 alongside diagnoses that already fully account for the back pain. For example, if the provider has also coded a lumbar disc herniation (M51.16) or lumbar radiculopathy (M54.16), adding M54.59 on the same claim triggers Excludes logic and creates edits. The structural code is the diagnosis; M54.59 becomes redundant and incorrect.
Use G89.29 as a Secondary Code for Chronic Cases
When the M54.59 presentation is chronic — meaning the pain has persisted for more than three months — consider adding G89.29 (Other chronic pain) as a secondary diagnosis. This supports medical necessity for ongoing treatment, especially in physical therapy and pain management settings. If the encounter is primarily for pain management (such as an injection visit), sequence G89.29 first.
Confirm Medicare and Commercial Payer Rules
Medicare’s National Coverage Determination for acupuncture in chronic low back pain includes M54.59 as an accepted diagnosis code in most MAC jurisdictions. However, payer-specific Local Coverage Determinations can vary. Always verify your MAC’s current LCD before submitting acupuncture claims with M54.59. Some commercial payers may also require imaging authorization for certain procedures when this code appears, particularly for injection therapies.
Check Your EHR and Superbill
If your practice’s charge capture system still shows M54.5 anywhere — without the fifth digit — fix it immediately. Every claim submitted with the old parent code in 2026 gets denied automatically. The fifth digit is not optional; it is required.
Match the CPT Code to the Clinical Picture
Different treatment settings pair different procedure codes with M54.59. In physical therapy, you will commonly see it alongside CPT codes for therapeutic exercise, manual therapy, and neuromuscular reeducation. For chiropractic settings, spinal manipulation codes (CPT 98940–98942) pair frequently with M54.59. In pain management, epidural steroid injection codes may pair with it, though payer authorization requirements vary — some carriers require imaging evidence for injections tied to soft-tissue diagnoses rather than vertebrogenic ones.
Related ICD-10 Codes You Need to Know
Coders working with other low back pain M54.59 should stay familiar with the surrounding code ecosystem to avoid missequencing and claim edits:
| Code | Description | When to Use Instead of M54.59 |
|---|---|---|
| M54.50 | Low back pain, unspecified | When documentation lacks any identified mechanism |
| M54.51 | Vertebrogenic low back pain | When MRI confirms Modic changes and provider documents vertebrogenic source |
| M54.41 / M54.42 | Lumbago with sciatica, right/left | When low back pain includes documented sciatic nerve involvement |
| M54.16 | Lumbar radiculopathy | When nerve root irritation is the primary documented finding |
| M51.16 / M51.17 | Lumbar disc herniation with myelopathy | When disc herniation is confirmed as the pain source |
| M51.36x | Lumbar disc degeneration | When disc degeneration is specifically documented as the etiology |
| M47.816 | Lumbar spondylosis without myelopathy | When spondylosis is the documented cause of pain |
| S39.012A | Low back strain, initial encounter | When a clear acute injury mechanism (like lifting) caused the pain |
| G89.29 | Other chronic pain | Secondary code for chronicity when pain exceeds three months |
Common Mistakes Coders Make with M54.59
After working with back pain coding for years, the same errors come up over and over again. Here is what to watch out for:
Treating M54.59 as a catch-all for everything that does not fit elsewhere. This code is not the trash bin of back pain coding. It requires a documented, specific, non-vertebrogenic pain mechanism. Using it vaguely undermines its clinical integrity and increases audit risk.
Using M54.59 when M54.50 is actually correct. If the clinical note genuinely says nothing more than “low back pain,” then M54.50 is the right call, not M54.59. Upcoding to M54.59 without documentation to support it is incorrect — and potentially fraudulent if done repeatedly.
Combining M54.59 with structural diagnosis codes that already explain the pain. As mentioned above, pairing M54.59 with disc herniation codes, radiculopathy codes, or spondylosis codes on the same claim creates Excludes logic violations. Pick the most accurate code and stick with it.
Still using the old M54.5 parent code. Submitting claims with M54.5 in 2026 is a guaranteed denial. There is truly no excuse for this error in 2026. Update your systems now.
Not updating the diagnosis code across the episode of care. As a patient’s condition evolves and more clinical information becomes available, the diagnosis code should be updated accordingly. A patient who initially receives M54.50 because their pain was uncharacterized may need to be updated to M54.59 at the next visit once the provider identifies a specific mechanism. Freezing the code from the first visit across all subsequent visits is inaccurate.
Skipping documentation queries. When the clinical note is ambiguous — where it hints at a mechanical or myofascial mechanism but does not explicitly state it — coders should query the provider rather than defaulting to M54.50. A simple clarification note can unlock M54.59 and produce a more accurate, supportable claim.
2026 Updates: What You Need to Know for M54.59 Right Now
The FY2026 ICD-10-CM cycle, effective October 1, 2025, did not change the code definition or structure of M54.59 itself. The code description remains “Other low back pain” and the billable status remains fully active through September 30, 2026. However, several important 2026 developments directly affect how this code gets used:
No structural code changes in FY2026 for M54. CMS confirmed that M54.50, M54.51, and M54.59 remain defined exactly as they have been since their 2021 introduction. No new subcategories, no deleted codes within M54 for this cycle.
Adjacent disc degeneration codes got more granular in FY2025, and those changes still apply in 2026. CMS introduced expanded sixth-character detail for lumbar disc degeneration (M51.36x) and lumbosacral disc degeneration (M51.37x) starting in FY2025. These distinguish between back pain only, leg pain only, combined patterns, and unspecified pain. Because M51.36x carries an Excludes1 relationship with certain M54.5x codes, coders must be careful not to pair M54.59 with M51.360 or M51.370 on the same claim.
April 1, 2026 mid-year update. The ICD-10-CM mid-year update, effective April 1, 2026, introduced several musculoskeletal code revisions. Coders should review updated crosswalk tables to confirm no new Excludes relationships have been created that affect M54.59 pairings.
Medicare acupuncture coverage still active. Medicare’s NCD for acupuncture in chronic low back pain continues in 2026, and M54.59 remains an accepted supporting diagnosis in most MAC jurisdictions. Coders billing acupuncture for chronic other low back pain should confirm their MAC’s specific covered diagnosis list annually.
AI coding tools are increasingly flagging M54.59 use patterns. More practices are deploying AI-assisted coding platforms in 2026 that automatically flag when M54.59 is used without adequate documentation support, or when it appears alongside conflicting structural codes. These tools are reducing denial rates significantly for practices that use them correctly.
Treatment Approaches for Other Low Back Pain
Understanding how M54.59 presentations typically get treated helps coders pair the right procedure codes and helps patients know what to expect. Since this code covers several distinct clinical patterns, treatment approaches vary:
Physical therapy is the first-line treatment for both mechanical and myofascial low back pain. Programs focus on muscle strengthening, flexibility, movement pattern correction, and trigger point release. Most patients with M54.59 presentations respond well to a structured PT program when the underlying mechanism is accurately identified and addressed.
Manual therapy and chiropractic care — including spinal manipulation, soft-tissue mobilization, and instrument-assisted techniques — are commonly used for mechanical and facet-mediated presentations. When the clinical notes support M54.59 and the exam documents findings that justify manipulation, chiropractic CPT codes pair cleanly with this diagnosis.
Trigger point injections are a targeted option for myofascial low back pain with documented trigger points. These are typically covered under procedure codes 20552 or 20553, and M54.59 serves as a supporting diagnosis, provided the documentation confirms the myofascial source.
Dry needling and acupuncture target trigger points and pain pathways in both myofascial and mechanical presentations. For Medicare beneficiaries with chronic other low back pain, acupuncture coverage applies when M54.59 is properly documented and meets chronicity criteria.
NSAIDs and muscle relaxants are commonly used for short-term symptom management in acute mechanical back pain. For chronic presentations, pain specialists may add low-dose tricyclic antidepressants or gabapentinoids to address the central sensitization component.
Frequently Asked Questions (FAQ)
What does M54.59 mean?
M54.59 is the ICD-10-CM diagnosis code for “Other low back pain.” It covers lower back pain presentations where the provider has identified a specific source or mechanism — such as myofascial, mechanical, or facet-related pain — that does not qualify as vertebrogenic (M54.51) and has no more precise ICD-10 code available.
When should you use M54.59 vs M54.50?
Use M54.50 when the clinical documentation only says “low back pain” with no further characterization. Use M54.59 when the provider documents a specific pain type or mechanism — like “mechanical low back pain” or “myofascial pain syndrome” — even if it does not rise to the level of a more specific structural code.
Is M54.59 a valid code in 2026?
Yes. M54.59 is fully active and billable in the FY2026 ICD-10-CM cycle, covering all claim dates from October 1, 2025 through September 30, 2026.
Can I still use M54.5 in 2026?
No. M54.5 (without a fifth digit) became a non-billable parent code on October 1, 2021. Claims submitted with M54.5 in 2026 will be automatically rejected. You must use M54.50, M54.51, or M54.59.
Can M54.59 and M54.50 appear on the same claim?
No. These codes represent different levels of specificity for the same condition. You pick the one that matches the documentation for that encounter. They cannot both appear as diagnoses for the same low back pain on a single claim.
Does M54.59 cover myofascial low back pain?
Yes. Myofascial low back pain is one of the clinical synonyms recognized for M54.59. When the provider documents paraspinal trigger points and a myofascial pain pattern, M54.59 is the appropriate diagnosis code.
What secondary code can I add for chronic other low back pain?
G89.29 (Other chronic pain) is the recommended secondary code when the M54.59 presentation has been present for more than three months and chronicity is documented in the chart.
Is M54.59 covered for Medicare acupuncture?
In most MAC jurisdictions, yes. Medicare’s NCD for acupuncture in chronic low back pain includes M54.59 as an accepted diagnosis code. Always verify your specific MAC’s current Local Coverage Determination before submitting, as policies can vary by jurisdiction.
The Bottom Line on M54.59
The M54.59 other low back pain code is genuinely useful — but only when documentation supports it. It sits right in the sweet spot between vague unspecified pain (M54.50) and the highly specific vertebrogenic category (M54.51). It rewards providers who take the time to characterize their patients’ pain and coders who read clinical notes carefully.
As payers continue tightening their scrutiny of musculoskeletal claims in 2026, getting this code right matters more than ever. Upgrade your documentation templates, ditch the old M54.5, train your coders on the M54.5x decision tree, and make sure every claim you submit for other low back pain actually tells the story the chart is telling.
That is how you keep claims clean, patients properly documented, and audits at bay — all the way through the end of FY2026 and beyond.
This article is written for informational and educational purposes for healthcare professionals and medical coders.