M54.2 — Cervicalgia ICD-10 Code
Neck pain hits harder than most people expect. It limits movement, kills productivity, and sends millions of Americans straight to their doctor every year. In fact, about one in three U.S. adults deals with neck pain at any given time, making it one of the most billed musculoskeletal complaints across every healthcare setting — from primary care to physical therapy to pain management.
So when a provider documents neck pain, the billing team immediately needs the right answer to a very specific question: what is M54.2? If you work in medical coding, you already know this code by heart. But if you are a provider, a patient, or someone newer to ICD-10 billing, this guide breaks everything down — clearly, accurately, and updated for 2026.
Let’s get into it.
What Is M54.2? The Full Meaning Behind the Code
The Official ICD-10-CM Definition
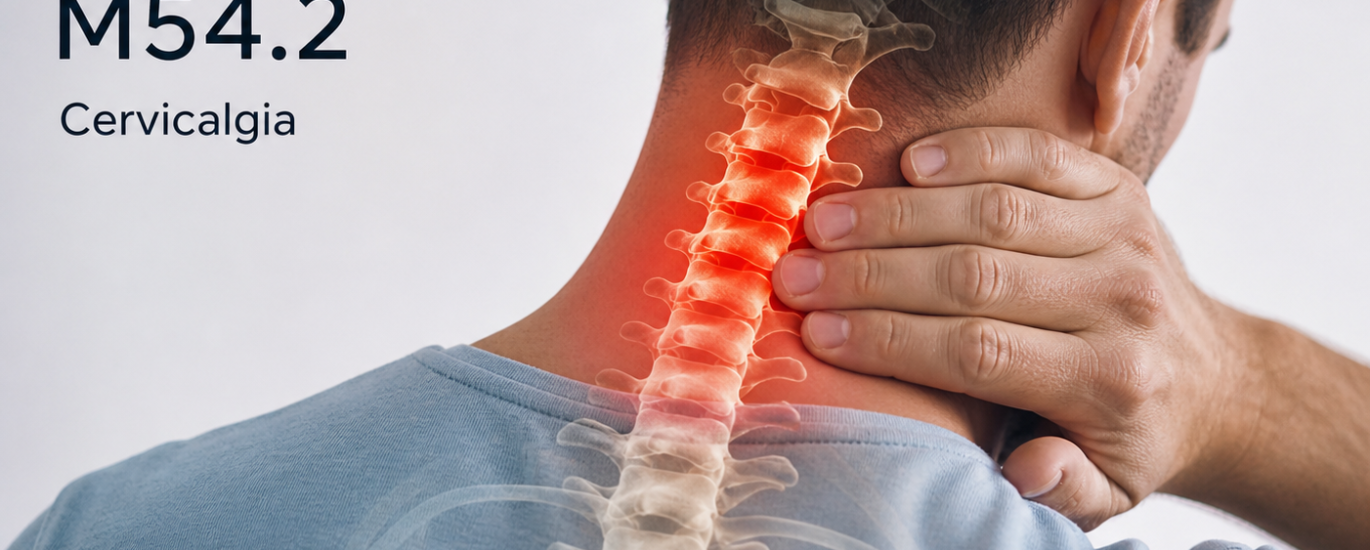
So, what does diagnosis code M54.2 mean exactly? In the simplest possible terms, M54.2 is the ICD-10-CM code for Cervicalgia — which is just the clinical term for neck pain. Specifically, it describes pain localized to the cervical spine (the neck region) that does not link to a more specific structural condition like a herniated disc, fracture, or nerve disorder.
The cervical spine runs from the base of the skull down to the upper chest, made up of seven vertebrae labeled C1 through C7. When someone experiences discomfort, stiffness, aching, or soreness anywhere in that region — without a clearly identified underlying pathology driving it — M54.2 is the code that captures it.
Clinicians and coders place M54.2 within ICD-10-CM Chapter 13, which covers Diseases of the Musculoskeletal System and Connective Tissue. More specifically, it falls under the M54 Dorsalgia category, the same family that houses thoracic and lumbar back pain codes.
What Is Cervicalgia M54.2 in Plain English?
If someone asks what is cervicalgia M54.2 in plain language, here is the honest answer: it means the patient has neck pain, and the provider cannot yet — or did not need to — pin it to a specific structural cause. The pain is real. It is localized to the neck. But it does not stem from something like a slipped disc or a pinched nerve, because if it did, a more specific code would take over.
Think of M54.2 as the clinically appropriate code for neck pain in its most straightforward form — mechanical, muscular, postural, or simply unspecified in origin.
Is M54.2 Billable in 2026?
Absolutely. The 2026 edition of ICD-10-CM M54.2 became effective on October 1, 2025. It covers HIPAA-covered transactions from October 1, 2025 through September 30, 2026. Providers across primary care, orthopedics, physical therapy, chiropractic care, neurology, and pain management all bill this code regularly. It is one of the most frequently submitted musculoskeletal diagnosis codes in the United States, appearing on more than 12 million medical claims annually.
Symptoms of Cervicalgia (M54.2)
What Patients Actually Feel
Patients presenting with cervicalgia typically describe a range of symptoms that vary in intensity and duration. Recognizing these helps providers document more accurately and gives coders the clinical support they need to justify M54.2 on a claim.
The most common symptoms include a dull, aching pain in the back or sides of the neck, stiffness or tightness that limits turning the head, a sharp or burning sensation with certain movements, muscle spasms in the neck and upper shoulders, tenderness when touching the neck muscles, and headaches that start at the base of the skull and move upward.
In some cases, the discomfort spreads to the shoulders or the upper back. Patients may also report difficulty sleeping, fatigue from constant tension, and trouble looking up or down for extended periods.
When Symptoms Push Beyond M54.2
Here is where coders need to pay close attention. When neck pain radiates down the arm — causing numbness, tingling, or weakness in the hand or fingers — that signals nerve root involvement. At that point, M54.2 no longer fits. The clinical picture now points toward cervical radiculopathy (M54.12) or a cervical disc disorder under the M50 series. The symptoms guide the code, so always read the full clinical note before selecting M54.2.
Common Causes of Cervicalgia
Muscle Strain and Poor Posture
Muscle strain tops the list of causes that land squarely under M54.2. Sitting at a desk for hours, looking down at a phone (commonly called “text neck”), working with improper ergonomics, or sleeping in an awkward position all create significant strain on the cervical muscles and ligaments. This type of mechanical neck pain typically shows no structural finding on imaging, making M54.2 a clean and appropriate fit.
Whiplash and Trauma
Whiplash injuries from car accidents, sports impacts, or sudden head movements frequently produce cervicalgia. As long as imaging does not reveal a fracture or structural cervical damage, M54.2 captures the diagnosis. If the injury ties to a specific trauma mechanism, coders should also consider adding an external cause code per ICD-10-CM guidelines.
Degenerative Conditions
Early-stage degenerative changes in the cervical spine — including mild disc wear and age-related joint changes — can contribute to neck pain even without nerve involvement. Importantly, once imaging confirms that a cervical disc disorder drives the pain, the M50 series codes replace M54.2. The Excludes1 rule makes this mandatory, not optional.
Inflammatory and Systemic Conditions
Inflammatory conditions like rheumatoid arthritis can produce neck pain, and systemic diseases sometimes manifest with cervical discomfort. In these cases, coders need to evaluate whether a more specific code better captures the underlying condition rather than defaulting to M54.2.
Stress and Myofascial Tension
Chronic stress causes people to unconsciously hold tension in the neck and shoulder muscles. Over time, this myofascial tension builds into consistent cervicalgia. Since no structural pathology drives it, M54.2 fits well — provided documentation supports the musculoskeletal nature of the pain.
M54.2 vs. Related Neck Pain Codes: Knowing the Difference
A lot of providers and coders wonder what is M54 2 versus the other neck and spine codes they see daily. The answer comes down to specificity. Here is a clear breakdown of where M54.2 ends and other codes begin.
When Disc Pathology Takes Over
M50 series — Cervical Disc Disorders handle any neck pain that cervical intervertebral disc problems drive:
- M50.0 — Cervical disc disorder with myelopathy (spinal cord compression)
- M50.1 — Cervical disc disorder with radiculopathy (nerve root involvement)
- M50.2 — Other cervical disc displacement (herniated disc without myelopathy or radiculopathy)
- M50.3 — Cervical disc degeneration
If imaging confirms that a disc issue causes the neck pain, switch from M54.2 to the appropriate M50 code. The Excludes1 note on M54.2 makes this non-negotiable.
When Nerve Pain Enters the Picture
M54.12 — Radiculopathy, Cervical Region applies when neck pain radiates into the arm due to nerve root compression. This is not the same condition as simple cervicalgia, and coders can actually use both M54.2 and M54.12 on the same claim if documentation supports both conditions independently. The AAPC has confirmed no Excludes1 restriction between these two codes.
Spondylosis and Structural Degeneration
M47.812 — Cervical Spondylosis without Myelopathy or Radiculopathy applies when degenerative joint changes in the cervical vertebrae drive the neck pain without nerve compression.
Spinal Stenosis
M48.02 — Spinal Stenosis, Cervical Region covers neck pain caused by narrowing of the spinal canal that compresses neural structures.
Trauma-Related Neck Injury
S13.4xxA — Sprain of Cervical Spine fits cases of acute neck injury from trauma — like whiplash from a car accident — rather than the more generalized cervicalgia that M54.2 covers.
Chronic Pain Modifier
G89.29 — Other Chronic Pain works as a secondary code alongside M54.2 when documentation clearly identifies the cervicalgia as chronic, typically defined as lasting beyond three months.
Psychogenic Neck Pain
F45.41 — Psychogenic Dorsalgia replaces M54.2 when psychological factors fully drive the neck pain. You cannot bill M54.2 and F45.41 together.
Billing Tips: How to Get M54.2 Claims Paid Right in 2026
This section matters the most to billers and coders who deal with real claims going out the door every day. Getting M54.2 right means clean submissions, faster payments, and fewer denials. Here is what to do.
Document the Pain With Precision
The provider’s note must go beyond “neck pain.” Strong documentation for M54.2 includes the pain’s location (posterior neck, lateral neck, bilateral), intensity level (mild, moderate, severe), quality (sharp, dull, aching, burning), duration (acute versus chronic), and any functional limitations. The more detail the note contains, the stronger the clinical justification for M54.2 and any associated procedures.
Specify Acute vs. Chronic Status
Documentation of whether the pain is acute or chronic directly affects treatment authorization and payer review. For chronic cervicalgia lasting more than three months, add G89.29 as a secondary code. This combination strengthens medical necessity for ongoing physical therapy, pain injections, or specialist referrals.
Pair the Right CPT Codes
M54.2 must align with the CPT codes on the same claim. Common CPT pairings include office visits (99202-99215 range), cervical imaging (72040 for X-ray, 72141 for MRI), physical therapy evaluations (97161-97163), trigger point injections (20552-20553), chiropractic manipulation (98940-98942), and therapeutic procedures. Payers scrutinize CPT-diagnosis mismatches, so the procedure must make clinical sense for cervicalgia.
Use Modifier -25 and Modifier -59 Correctly
When a provider performs a significant evaluation and management service on the same day as a procedure, Modifier -25 attaches to the E/M code to signal a separately identifiable service. When two distinct procedural services occur on the same day, Modifier -59 applies. These modifiers help prevent bundling denials on multi-service claims.
Never Bill M54.2 When a Disc Disorder Drives the Pain
The Excludes1 rule is absolute: M54.2 and M50 codes cannot appear together on the same claim for the same condition. If the provider documents a cervical disc disorder as the cause of neck pain, use the M50 code. Submitting both triggers an automatic denial.
Keep Diagnosis Codes Consistent Across the Episode of Care
If a patient returns for follow-up visits and the code switches from M54.2 to a more specific code without documentation supporting the change, payers will question the encounter. Update the diagnosis code only when clinical documentation clearly supports a more specific finding.
Common Coding Mistakes with M54.2 (And How to Fix Them)
Mistake 1: Using M54.2 When a Disc Disorder Is Documented
This ranks as the single most costly M54.2 error. The moment the provider confirms a cervical disc disorder as the cause of the neck pain, the claim must use the M50 series. Using M54.2 instead violates the Excludes1 rule and guarantees a denial.
Mistake 2: Missing the Radiculopathy Code When Arm Symptoms Exist
When a patient reports neck pain that radiates into the arm with numbness or tingling, the clinical picture includes radiculopathy. Coders who stick with M54.2 alone miss M54.12, which more accurately captures the full clinical presentation and often affects treatment authorization.
Mistake 3: Vague Documentation That Cannot Support the Code
Writing “neck pain” in the chart and nothing else is not enough. Without details about duration, intensity, location, and absence of more specific diagnoses, the documentation does not defend M54.2 during a payer audit. Educate providers to document the clinical reasoning behind their code selection.
Mistake 4: Failing to Add G89.29 for Chronic Cases
For patients with long-standing cervicalgia, skipping G89.29 as a secondary code misses an opportunity to demonstrate medical necessity for continued or escalating treatment. This omission frequently triggers authorization denials for pain management services.
Mistake 5: Confusing M54.2 With Cervical Spondylosis
When imaging reveals cervical spondylosis as the underlying cause of neck pain, M47.812 fits better than M54.2. Using M54.2 in this scenario understates the clinical complexity and may reduce appropriate reimbursement.
Mistake 6: Ignoring Laterality Documentation
Some payers and specialty guidelines expect documentation of whether the neck pain is right-sided, left-sided, or bilateral. Although M54.2 itself does not have laterality-specific subcodes, clinical notes should still capture laterality when the provider identifies it. Missing this detail can complicate secondary coding and authorization requests.
2026 ICD-10-CM Updates Affecting M54.2
What Stayed the Same
Good news for coders: M54.2 itself did not undergo structural changes in the FY2026 ICD-10-CM update cycle. The code remains billable, specific, and valid under its existing definition as of October 1, 2025. Its classification under the M54 Dorsalgia category, its Excludes1 relationship with M50 codes, and its MS-DRG groupings all stayed intact.
Changes in the Broader M54 and M50 Neighborhood
While M54.2 held steady, surrounding codes saw continued refinement. The M50 cervical disc disorder family continues to expand in clinical specificity, which means coders need sharper documentation to correctly distinguish between M54.2 cervicalgia and M50 series conditions. Payers increasingly scrutinize claims where M54.2 appears alongside imaging results that might support a more specific M50 code.
Expanded Excludes1 Monitoring
The FY2026 update cycle brought expanded attention to Excludes1 relationships across the musculoskeletal chapter. CMS and NCHS clarified bundling logic in several adjacent code families. Although M54.2 itself was not part of these clarifications, coders billing neck pain alongside cervical disc or radiculopathy codes should verify the Excludes1 and Excludes2 relationships with each encounter before submitting.
The Telehealth and Remote Monitoring Impact
In 2026, telehealth remains a major delivery channel for managing cervicalgia, especially for patients in rural areas or those receiving physical therapy remotely. Documentation for telehealth-based cervicalgia encounters must meet the same specificity requirements as in-person visits. Coders billing M54.2 on telehealth claims should pair it with the appropriate place-of-service code and confirm payer-specific telehealth billing rules, as Medicare and commercial payers continue to update their guidance.
Frequently Asked Questions (FAQ)
What does diagnosis code M54.2 mean on my paperwork? M54.2 is the ICD-10 code for cervicalgia, which simply means neck pain. Your provider used this code to document that you have pain localized to the cervical spine (your neck), and the pain does not link to a more specific condition like a herniated disc or pinched nerve. It does not mean something serious is necessarily wrong — often it just captures mechanical or muscular neck pain.
What is cervicalgia M54.2 in simple terms? Cervicalgia is the medical term for neck pain. M54.2 is the billing code that represents it. When your doctor writes M54.2 on your chart, they are documenting that your neck hurts without tying it to a specific structural diagnosis.
What is M54 2 — is it the same as a neck injury? Not necessarily. M54.2 covers general neck pain, which can come from muscle strain, poor posture, stress, or minor trauma. A neck injury with a confirmed structural cause — like a fracture or disc rupture — would use a different, more specific ICD-10 code.
Can M54.2 and M54.12 appear on the same claim? Yes. M54.12 covers cervical radiculopathy (nerve root pain radiating down the arm), and M54.2 covers localized neck pain. Because no Excludes1 restriction exists between them, you can bill both when clinical documentation supports both conditions independently.
Can you use M54.2 for chronic neck pain? Yes. M54.2 works for both acute and chronic cervicalgia. When the pain is chronic (lasting longer than three months), add G89.29 as a secondary diagnosis code. This combination better supports medical necessity for extended treatment plans.
Is M54.2 billable by chiropractors and physical therapists? Absolutely. M54.2 is billable across multiple specialties including primary care, orthopedics, chiropractic, physical therapy, neurology, and pain management. Each specialty may pair it with different CPT codes based on the services they provide.
What happens if I use M54.2 when a disc disorder is confirmed? The claim will likely get denied. The Excludes1 rule on M54.2 prohibits using it when a cervical intervertebral disc disorder drives the pain. In that case, the M50 series takes over.
What is the difference between M54.2 and M54.12? M54.2 covers localized neck pain (cervicalgia) without nerve involvement. M54.12 covers cervical radiculopathy, meaning the neck pain radiates down the arm because of nerve root compression. They describe different clinical presentations and coders can use both when documentation supports both.
Final Word: Master M54.2 and Keep Your Neck Pain Claims Clean
Understanding what is diagnosis code M54.2 gives every provider, coder, and biller a meaningful edge. This one code powers millions of claims every year across every practice setting that treats neck pain — and doing it right makes a measurable difference in reimbursement, compliance, and clinical accuracy.
The core rules are simple: use M54.2 when the documentation supports localized cervical pain without a disc disorder as the cause, document with specificity every single time, add G89.29 when chronic pain enters the picture, and always respect the Excludes1 relationship with M50 codes.
As 2026 continues, payers keep raising the documentation bar. They want specificity. They want clinical support. And they will deny claims where M54.2 appears without the documentation muscle to back it up.
Stay sharp. Code with precision. And when the clinical picture shows you something more specific than simple neck pain, follow the evidence and pick the right code.
This article provides educational information for medical coders, billers, healthcare providers, and patients. Always verify all coding decisions against the official ICD-10-CM FY2026 guidelines published by CMS and NCHS, as well as payer-specific policies.