If you handle endocrinology billing, primary care coding, or any practice that sees diabetic patients regularly, the e11.65 diagnosis code comes up constantly. And yet it is one of the most misused codes in the entire ICD-10 system. Coders either default to E11.9 out of habit, or they apply E11.65 without proper documentation to back it up. Both mistakes cost real money, and both are completely avoidable.
This guide covers everything you need to know about the e11.65 ICD-10 code in 2026, from what it actually means clinically, to the symptoms it captures, the causes it reflects, and exactly how to use it correctly for billing without triggering denials or audits.
What E11.65 Means: Breaking Down the Diagnosis Code
E11.65 is the official ICD-10-CM diagnosis code for Type 2 diabetes mellitus with hyperglycemia. It sits within Chapter 4 of the ICD-10 tabular list, which covers endocrine, nutritional, and metabolic diseases (E00 through E89). More specifically, it falls under the E11 category, which covers all Type 2 diabetes mellitus presentations.
Here is the clinical breakdown of that code structure:
- E = Endocrine, nutritional, and metabolic diseases
- E11 = Type 2 diabetes mellitus
- E11.6 = Type 2 diabetes mellitus with other specified complications
- E11.65 = Type 2 diabetes mellitus with hyperglycemia specifically
So when you see E11.65, you are looking at a patient with icd 10 diabetes type 2 who also has a documented episode of elevated blood glucose during the current encounter. The ICD-10-CM system treats hyperglycemia not as a routine finding but as a complication of diabetes. That is why it sits in the E11.6 “other specified complications” subcategory rather than under the basic E11.9 unspecified code.
The 2026 edition of ICD-10-CM E11.65 became effective on October 1, 2025, and remains valid through September 30, 2026. It has been a billable and specific code every year since ICD-10 first launched in 2016, and it has not changed in definition, making it one of the most stable codes in the diabetes category.
One critical thing to understand right away: ICD-10-CM presumes a cause-and-effect relationship between Type 2 diabetes and hyperglycemia. That means the physician does not need to explicitly write “hyperglycemia caused by diabetes” in the note. If both conditions are documented in the assessment, you can apply E11.65. This presumed linkage makes the icd 10 code for hyperglycemia in a Type 2 diabetic patient straightforward to apply when documentation is solid.
Symptoms of Hyperglycemia in Type 2 Diabetes Patients
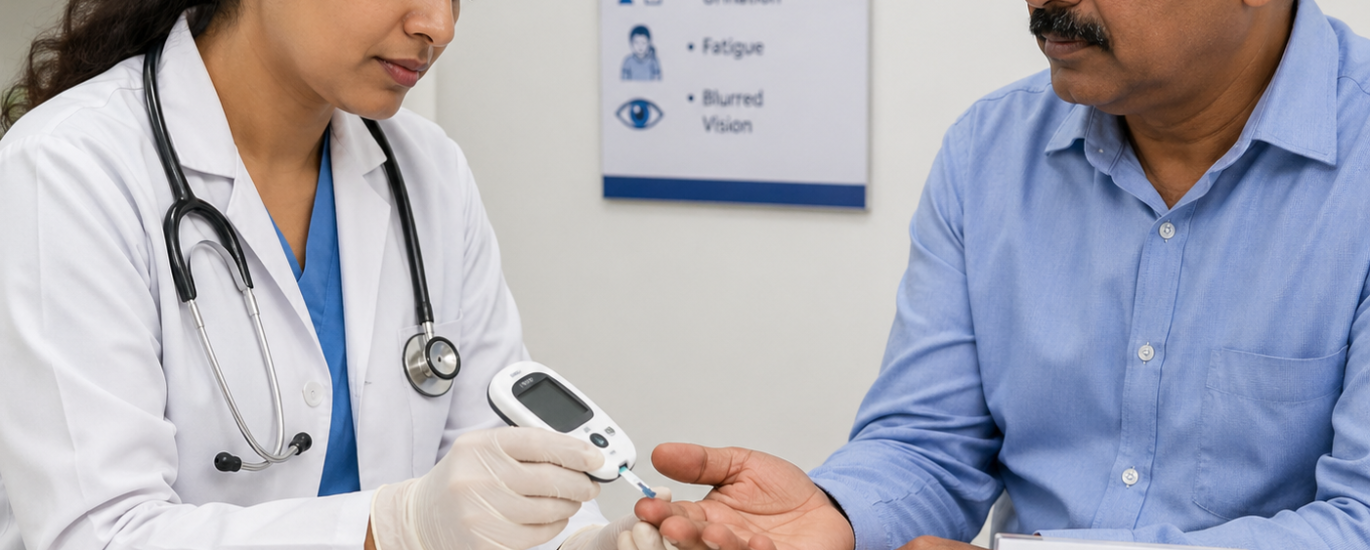
Understanding what hyperglycemia looks like clinically helps coders recognize when E11.65 is the right code and helps providers write stronger supporting documentation. Patients experiencing high blood sugar episodes typically present with:
Excessive thirst (polydipsia) – The kidneys work overtime trying to flush excess glucose through urine, pulling fluid from body tissues and triggering intense, persistent thirst.
Frequent urination (polyuria) – Elevated glucose spills into the urine, dragging water along with it. Patients notice they are getting up multiple times a night or running to the bathroom far more than usual.
Fatigue and low energy – When glucose cannot enter cells properly, the body lacks its primary fuel source. Even basic tasks feel exhausting.
Blurred vision – High blood sugar causes fluid shifts in the lenses of the eyes, temporarily distorting focus. This is one of the most common complaints during hyperglycemic episodes.
Slow-healing wounds or infections – Elevated glucose impairs immune function and circulation, making even small cuts or infections take much longer to resolve.
Headaches – Dehydration caused by glucose-driven fluid loss often triggers persistent head pain.
Difficulty concentrating – Sometimes called “brain fog,” this happens because glucose metabolism in the brain is disrupted during hyperglycemic episodes.
Nausea – In more significant episodes, patients may feel sick to their stomach, particularly when blood sugar climbs into very high ranges.
Importantly, when these symptoms are documented as part of the encounter for a Type 2 diabetic patient, they support the use of E11.65. However, you do not need to separately code the symptoms. Per ICD-10-CM guidelines, symptoms that are integral to the coded condition, like polyuria or polydipsia in the context of hyperglycemia, should not receive their own additional codes.
What Causes Hyperglycemia in Type 2 Diabetes Patients
Knowing the triggers helps both clinically and from a coding standpoint, because the cause often determines whether additional secondary codes are appropriate. Common causes of hyperglycemic episodes in Type 2 diabetes include:
Medication non-compliance – Skipping oral hypoglycemic medications, missing insulin doses, or taking incorrect amounts is the number one trigger. Documentation of non-compliance supports the use of Z91.19 as a secondary code.
Dietary factors – Consuming high-carbohydrate or high-sugar meals causes rapid glucose spikes, especially when the patient is on a fixed medication regimen that cannot compensate fast enough.
Illness and infection – Any stress on the body, including upper respiratory infections, urinary tract infections, or pneumonia, raises cortisol and other stress hormones that push blood glucose up. Code the infection separately as an additional diagnosis.
Physical inactivity – Muscle tissue is a major glucose absorber. When patients reduce physical activity, glucose clearance slows and levels rise.
Medication interactions or new prescriptions – Corticosteroids, certain antipsychotics, and even some blood pressure medications can raise blood glucose significantly. If a drug is identified as the cause, consider whether E09 (drug or chemical induced diabetes) is more appropriate than E11.65.
Insulin resistance progression – As Type 2 diabetes advances, the body’s cells become increasingly resistant to insulin’s effects, making blood sugar harder to control even with medication.
Hormonal changes – Conditions like Cushing’s syndrome or polycystic ovary syndrome (PCOS) can worsen insulin resistance. Code any confirmed associated endocrine disorder separately.
Emotional or physical stress – Stress hormones like adrenaline and cortisol have well-documented blood sugar-raising effects. Major surgery, trauma, or severe psychological stress can tip a stable diabetic patient into a hyperglycemic episode.
E11.65 vs. E11.9 vs. E11.40: Picking the Right Code
This is where the real coding decisions happen. These three codes get confused constantly, and mixing them up is one of the top causes of diabetes claim denials.
E11.65 vs. E11.9
E11.9 is the icd 10 diabetes type 2 code for patients with no documented complications. It is the right code when a patient comes in for routine diabetes management, their glucose is well-controlled, and the physician’s note does not mention any current complications.
E11.65 applies when the physician’s assessment explicitly documents hyperglycemia during the current encounter. The visit notes must show elevated glucose, reference to “poorly controlled” or “out of control” diabetes, or directly state hyperglycemia as part of the assessment. Without that documentation, you cannot apply E11.65 even if the patient has a history of poor control.
Think of it this way: E11.9 is the stable, routine visit code. E11.65 is the “blood sugar is a problem today” code. Applying one when the other is appropriate is a compliance issue, not just a billing preference.
E11.65 vs. E11.40
E11.40 is the code for Type 2 diabetes mellitus with diabetic neuropathy, unspecified. A patient can absolutely have both neuropathy and hyperglycemia at the same time. In fact, they often do. When both conditions are documented during the same encounter, you code both E11.65 and E11.40. These are not mutually exclusive.
However, never assume neuropathy just because a patient has long-standing diabetes. The physician must explicitly document the neuropathy diagnosis. And if the documentation specifies the type of neuropathy, such as peripheral polyneuropathy, use E11.42 instead of the unspecified E11.40.
2026 Updates: What Every Coder Needs to Know Right Now
The 2026 ICD-10-CM edition became effective October 1, 2025. While E11.65 itself did not change in this cycle, several important updates surround it that directly affect how you code Type 2 diabetes in 2026.
The new E11.A code for diabetes remission. This is the biggest change for Type 2 diabetes coding in recent years. E11.A officially represents Type 2 diabetes in remission, defined by the ADA as an A1C below 6.5% for at least three consecutive months without diabetes medication. When a patient previously coded with E11.65 achieves remission, you switch to E11.A. If remission breaks down and hyperglycemia returns, you switch right back to E11.65. Coders need to monitor this actively across encounters.
Tighter specificity expectations from payers. Medicare Advantage plans and major commercial insurers including UnitedHealthcare and Aetna have tightened their documentation requirements for diabetes claims in 2026. They now expect A1C values, treatment modalities, and specific complication assessments in notes before they will approve complex coding. A note that just says “diabetes with high glucose” without supporting lab values is a denial waiting to happen.
HCC risk adjustment scrutiny is up. Diabetes codes including E11.65 feed directly into Hierarchical Condition Category (HCC) risk adjustment models. Inaccurate or vague coding affects how practices are reimbursed under value-based care contracts. CMS has increased its focus on HCC accuracy, making clean E11.65 documentation more financially critical than ever.
The “questionable admission diagnosis” flag. E11.65 carries a “Questionable as Admission Dx” designation in the 2026 MS-DRG system. This means that if hyperglycemia alone is listed as the primary reason for inpatient admission, auditors will scrutinize whether the admission was medically necessary. Coders in hospital settings need to make sure the primary diagnosis truly drives the admission, with E11.65 sequenced accordingly.
Billing Tips for E11.65: How to Get Claims Approved the First Time
These practical steps will keep your E11.65 claims clean and your reimbursements timely.
Step 1: Confirm Documentation Before You Code
Never assume hyperglycemia. The physician’s assessment section must reference it, whether as “hyperglycemia,” “poorly controlled diabetes,” “out of control blood sugar,” or a clear clinical narrative describing elevated glucose levels. If it shows up only in the vitals or lab results without appearing in the assessment, query the provider before assigning the code.
Step 2: Always Add Z-Codes for Medications
This is one of the most skipped steps in diabetes coding and one of the most audit-generating omissions. When you apply E11.65, also add Z79.4 for long-term insulin use, Z79.84 for long-term oral hypoglycemic drug use such as metformin, glipizide, or newer SGLT2 inhibitors, and both Z codes when the patient uses both types.
Step 3: Code Every Documented Complication
If a patient has E11.65 plus documented diabetic retinopathy, neuropathy, or nephropathy, code every single one. The ICD-10 system is built for combination coding. Leaving out documented complications is under-coding and directly reduces your HCC risk score.
Step 4: Skip Separate Symptom Codes
Polydipsia, polyuria, fatigue, and blurred vision tied to the documented hyperglycemia do not need their own codes. They are integral to E11.65, and adding them separately can flag the claim for over-coding review.
Step 5: Back Every Claim with Lab Values
A1C results, fasting glucose readings, or random glucose values documented alongside the physician’s assessment create a rock-solid audit trail. Claims without supporting lab data face a much higher rate of secondary review.
Step 6: Update Codes at Every Single Encounter
Diabetes management is dynamic. A patient coded as E11.9 last visit who now presents with documented hyperglycemia must flip to E11.65 for the current visit. Running the same code visit after visit without re-evaluating current status is a compliance red flag that auditors notice quickly.lag.
Related Codes You Need in Your Daily Toolkit
Working with E11.65 regularly means you will routinely need these companion codes:
| Code | Description |
|---|---|
| E11.9 | Type 2 diabetes mellitus without complications |
| E11.40 | Type 2 diabetes with diabetic neuropathy, unspecified |
| E11.42 | Type 2 diabetes with diabetic polyneuropathy |
| E11.22 | Type 2 diabetes with diabetic chronic kidney disease, stage 1-2 |
| E11.649 | Type 2 diabetes with hypoglycemia without coma |
| E11.69 | Type 2 diabetes with other specified complication |
| E11.A | Type 2 diabetes mellitus in remission (new for FY2026) |
| E11.84 | Type 2 diabetes with hypoglycemia without coma (alternative) |
| Z79.4 | Long-term (current) use of insulin |
| Z79.84 | Long-term (current) use of oral hypoglycemic drugs |
| R73.09 | Other abnormal glucose (for borderline cases without confirmed diabetes diagnosis) |
| N18.3 | Chronic kidney disease, stage 3 |
| Z87.39 | Personal history of other endocrine diseases |
Common Mistakes That Get E11.65 Claims Denied
These are the errors coders make over and over with this code. Every single one is fixable with better documentation habits and a sharper review process.
Mistake 1: Using E11.9 when E11.65 applies.
If the physician’s note documents hyperglycemia but the coder submits E11.9, that is under-coding. Payers can catch this through algorithmic claims review, especially when lab results showing elevated glucose are also submitted. This creates a documentation contradiction that triggers audits.
Mistake 2: Using E11.65 when glucose is controlled.
The opposite error is just as problematic. Applying E11.65 to a visit where the patient’s A1C is 6.8%, glucose is stable, and the physician does not mention any elevation is over-coding. This is a compliance violation under HIPAA coding standards.
Mistake 3: Forgetting Z-codes for medications.
Submitting E11.65 without Z79.4 or Z79.84 when the patient is on diabetes medications creates a red flag. Payers see an active hyperglycemia code without any treatment documentation and question the claim’s clinical validity.
Mistake 4: Not coding all complications together.
Patients with E11.65 often also have neuropathy, retinopathy, or nephropathy. Leaving those out is both clinically inaccurate and financially harmful. Each documented complication has its own HCC value, and skipping it means your practice is not getting paid for the complexity of care it is actually providing.
Mistake 5: Confusing E11.65 with E11.69.
E11.69 covers “other specified complications” of Type 2 diabetes that do not have their own specific code. Hyperglycemia has its own specific code, which is E11.65. Using E11.69 when hyperglycemia is documented is the wrong code, plain and simple.
Mistake 6: Applying E11.65 without physician documentation.
Seeing a glucose reading of 280 in the lab panel does not automatically justify E11.65. The physician must address that reading in the assessment section of the note. If they do not, query the provider. If they will not update the note, you cannot apply the code.
Mistake 7: Never updating to E11.A when remission occurs.
With the new E11.A code active since October 2025, practices need to track remission eligibility. Continuing to code E11.65 for a patient who has been off medications with A1C under 6.5% for three months or more is inaccurate and potentially problematic during risk adjustment audits.
Frequently Asked Questions (FAQ)
What exactly is the E11.65 diagnosis code used for?
E11.65 is the ICD-10-CM code for Type 2 diabetes mellitus with hyperglycemia. You apply it when a physician documents that a Type 2 diabetic patient currently has elevated blood glucose, whether described as hyperglycemia, poorly controlled diabetes, or out of control blood sugar, during a specific encounter.
How is E11.65 different from E11.9?
E11.9 covers Type 2 diabetes without complications for stable, routine visits. E11.65 applies specifically when hyperglycemia is documented during the current encounter. The distinction hinges entirely on whether the physician’s note addresses elevated glucose as an active clinical issue during that visit.
Do I need to separately code the symptoms of hyperglycemia?
No. Symptoms like excessive thirst, frequent urination, and fatigue that are directly tied to the documented hyperglycemia should not be coded separately. ICD-10-CM treats these as integral to E11.65.
What Z-codes should I add alongside E11.65?
Always include Z79.4 for patients on insulin and Z79.84 for patients on oral hypoglycemic medications. Add both if the patient uses both types. These Z-codes are not optional; they are required coding instructions under ICD-10-CM guidelines.
Can I code E11.65 and E11.40 together?
Absolutely, yes. When a patient has both documented hyperglycemia and documented diabetic neuropathy during the same encounter, both codes apply. Multiple complications should all be coded when the documentation supports them.
Is the E11.65 code valid for 2026?
Yes. The 2026 edition of E11.65 became effective October 1, 2025, and remains valid through September 30, 2026. The code has not changed in description since it was introduced in 2016.
What is the new E11.A code and how does it relate to E11.65?
E11.A is a brand-new 2026 code for Type 2 diabetes in remission. When a patient previously coded with E11.65 achieves remission (A1C below 6.5% for 3+ months off all diabetes medications), you switch to E11.A. If their condition worsens and hyperglycemia returns, you return to E11.65.
Does the physician have to explicitly link diabetes and hyperglycemia?
No. ICD-10-CM presumes a causal relationship between Type 2 diabetes and hyperglycemia. If both are documented in the assessment, you can assign E11.65 without requiring the physician to state “hyperglycemia due to diabetes” in so many words.
What happens if I use E11.65 without documentation?
Applying E11.65 without the physician documenting hyperglycemia in the assessment is over-coding. This creates compliance risk, potential audit exposure, and possible repayment obligations if discovered during a payer audit.
The Bottom Line on E11.65 in 2026
The type 2 diabetes with hyperglycemia icd 10 code space is more tightly scrutinized in 2026 than it has ever been. CMS, Medicare Advantage plans, and commercial insurers are all watching diabetes coding with a sharper eye because of its direct impact on HCC risk scores and value-based payments.
Getting E11.65 right is not complicated, but it does require discipline. The physician needs to document hyperglycemia in the assessment. You need to add the right Z-codes for medications. You need to code every documented complication alongside it. And you need to stay current with changes like the new E11.A remission code.
Do all of that consistently, and your diabetes claims will be cleaner, your reimbursements faster, and your practice protected from the kind of audit exposure that keeps billing managers up at night. Skip those steps, and you are leaving money on the table while taking on compliance risk at the same time.
In diabetes coding, specificity is not optional. It is the job.