So your provider just handed you a paper that says M54.12, or maybe you are a coder staring at this code on a claim and wondering if you are using it right. Either way — you landed in the right place.
This guide breaks down everything you need to know about M54.12: what it means, why it matters in 2026, how to use it correctly for billing, and what patients can do to manage cervical radiculopathy without messing up their recovery. Whether you are a healthcare provider, a medical biller, or a patient who just got diagnosed, this article was built for you.
What Does ICD-10 Code M54.12 Mean?
Let us keep it simple. M54.12 is the official ICD-10-CM diagnosis code for Radiculopathy, Cervical Region — more commonly called cervical radiculopathy.
Here is what each character in the code actually tells you:
- M = Musculoskeletal system and connective tissue (ICD-10 Chapter 13)
- 54 = Dorsalgia (spine-related pain conditions)
- .1 = Radiculopathy (compressed or irritated nerve root)
- 2 = Cervical region (the neck)
So when you see M54.12, it literally translates to: a nerve root in the neck is being pinched or irritated, causing symptoms that radiate outward.
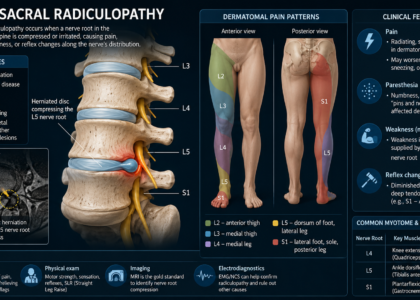
Think of your cervical spine as a stack of seven bones — vertebrae C1 through C7. Between each bone, nerve roots branch off and travel down into your shoulders, arms, and fingers. When something presses on one of those roots — a disc bulge, a bone spur, or arthritic narrowing — you get cervical radiculopathy. That is exactly what M54.12 is documenting.
Quick Answer: What does ICD-10 code M54.12 mean? M54.12 stands for Radiculopathy, Cervical Region. It codes for nerve root compression or irritation in the neck, causing pain, numbness, tingling, or weakness that radiates down the arm.
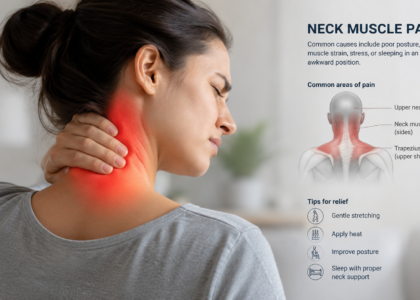
Symptoms Associated with M54.12
Patients who carry the M54.12 diagnosis code typically show up with a recognizable pattern. Here is what to look for clinically:
- Sharp or burning neck pain that shoots down one arm
- Numbness or tingling in the shoulder, arm, hand, or fingers
- Muscle weakness in the arm or grip
- Loss of deep tendon reflexes in the affected arm
- Pain that worsens with neck rotation or extension
- Temporary relief when placing the hand on top of the head (this reduces traction on the irritated nerve root)
One thing that surprises many providers — and patients too — is that the neck itself may not hurt very much at all. The radiating arm pain or hand tingling is often the loudest complaint. That is still M54.12 territory, as long as the source is a compressed cervical nerve root.
Symptoms frequently worsen at night, which is why so many people search how to sleep with cervical radiculopathy. We cover that in full detail below.
Causes of Cervical Radiculopathy
Before a provider confidently assigns the ICD-10 code for cervical radiculopathy, they need to understand what is driving the nerve compression. Common causes include:
Herniated or bulging disc — The disc’s inner material pushes outward and presses against a nearby nerve root. This is the most common cause in adults under 50.
Degenerative disc disease — Discs naturally shrink and lose height over time, narrowing the space where nerve roots exit. More common in adults over 50.
Bone spurs (osteophytes) — Cervical arthritis triggers bony overgrowths that crowd the neural foramen and compress nerve roots.
Spinal stenosis — Overall narrowing of the spinal canal can compress multiple nerve roots simultaneously.
Trauma or whiplash — Sudden injury can immediately compress or stretch a nerve root.
Poor posture — Prolonged forward head posture from desk work, phone use, or gaming gradually loads the cervical discs and stresses the nerve roots.
Why does the cause matter for coding? Because if a confirmed disc disorder is driving the radiculopathy, you need a different code entirely. More on that in the related codes and common mistakes sections.
M54.12 Billing Tips: What Every Coder Needs to Know in 2026
This is where most of the confusion lives. So let us walk through it clearly.
When Is M54.12 Billable?
M54.12 is a billable diagnosis code valid during the current fiscal year for HIPAA-covered transactions from October 1, 2025 through September 30, 2026. It falls under MS-DRG v43.0, grouped within codes 073 and 074 (Cranial and Peripheral Nerve Disorders).
Use M54.12 when:
- The provider’s assessment explicitly documents radiculopathy in the cervical region
- Symptoms are nerve-based — pain, numbness, tingling, or weakness — originating from the neck
- There is no confirmed cervical disc disorder as the underlying cause (see Excludes 1 rules below)
What Does Good Documentation Look Like?
Documentation of the diagnostic criteria met, the symptoms observed, and any supporting imaging studies in the assessment portion of the note is strongly encouraged. While comprehensive documentation supports the use of M54.12, it is not strictly necessary for physician billing.
That said, strong documentation protects you from audits. A solid note includes:
- Symptom description with anatomical location
- Physical exam findings like a positive Spurling’s test, dermatomal sensory changes, or reflex deficits
- Any imaging performed, along with clinical correlation to the findings
- Duration and progression of symptoms
Here is the key takeaway: even if an MRI comes back without a clear herniation, M54.12 can still be appropriate. If symptoms and exam — positive Spurling’s test, tingling in a dermatomal pattern, MRI showing mild disc bulge without definitive compression — point to nerve irritation, M54.12 is a correct and defensible code choice.
Can You Bill M54.50 and M54.12 Together?
Yes — in most situations you absolutely can. M54.50 covers low back pain (unspecified) and M54.12 covers cervical radiculopathy. Since these involve completely different anatomical regions, there is no Excludes 1 restriction between the two codes, and they can coexist on the same claim when both conditions are clearly and separately documented in the provider’s note.
Before you do this, always verify:
- Payer-specific bundling rules — some commercial payers have their own edits
- That each condition gets its own separate documentation in the assessment
- That M54.50 is truly the right lumbar code and not a more specific one like M54.51
Related ICD-10 Codes: Know the Difference
Knowing when not to use M54.12 is just as important as knowing when to use it. Here is a quick reference:
M54.10 — Radiculopathy, site unspecified. Use this only when the spinal region is not documented.
M54.12 — Radiculopathy, cervical region. Your go-to code for pinched nerve in the neck.
M50.1x — Cervical disc disorder with radiculopathy. Use this when a confirmed disc disorder is the cause — this is a combination code and replaces M54.12 entirely.
M47.2x — Spondylosis with radiculopathy. Use when arthritis is the confirmed driver.
M54.2 — Cervicalgia. Neck pain only, no nerve radiation.
M54.50 — Low back pain, unspecified. Completely separate region.
The critical rule to memorize: radiculopathy with cervical disc disorder (M50.1) and radiculopathy with spondylosis (M47.2) are both Excludes 1 exclusions from M54.12. If either of those conditions is confirmed, you must use the corresponding combination code — not M54.12.
Common Mistakes When Using M54.12
Even experienced coders and providers make these errors. Here are the ones that show up most often in audits and denials:
Mistake 1: Using M54.12 when a disc disorder is confirmed Once imaging or clinical findings confirm a herniated or displaced disc is compressing the nerve, you move to M50.1x. M54.12 and M50.1x are mutually exclusive.
Mistake 2: Defaulting to M54.10 (unspecified) when the cervical region is documented Specificity protects your claim. If the note says cervical radiculopathy, M54.12 is available and you should use it. Using non-specific codes when specific ones apply invites audits and downcoding.
Mistake 3: Skipping laterality documentation M54.12 does not distinguish left from right. Some payers accept that without issue. Others will deny if the side is not specified. Get in the habit of documenting which side is affected in every note — it takes two seconds and prevents headaches later.
Mistake 4: Confusing M54.2 (cervicalgia) with M54.12 Cervicalgia is pure neck pain. Cervical radiculopathy is nerve pain that travels. If a patient has a stiff, achy neck with zero radiation, M54.2 is the call. If there is arm numbness, tingling, or weakness — that is M54.12 territory.
Mistake 5: Using M54.12 when spondylosis is confirmed Arthritis-driven radiculopathy goes to M47.2x, not M54.12. The Excludes 1 note is explicit on this.
How to Sleep with Cervical Radiculopathy
This is genuinely one of the most-searched questions around this condition. Nighttime symptoms are brutal for a lot of people — and there is a clinical reason for it. Cortisol, the body’s primary anti-inflammatory hormone, reaches its lowest levels between midnight and 4 a.m., meaning the inflammation around a compressed nerve root has less opposition during the hours when a person is also lying still. That combination of reduced anti-inflammatory activity and sustained mechanical compression creates the perfect conditions for nighttime flares.
Here is what actually helps:
Back sleeping is generally the safest position. Use a cervical contour pillow to keep the neck in neutral alignment and the neural foramen as open as possible. This is the position physical therapists recommend most consistently.
Side sleeping can work with the right setup. Use one pillow for back sleepers or two for side sleepers, making sure not to bend the neck too far forward. Critically, avoid sleeping on the affected side — that compresses the irritated nerve root directly.
Stomach sleeping is the worst option. Stomach sleeping forces sustained neck rotation, which narrows the neural foramen on the rotated side and worsens arm symptoms.
Additional bedtime strategies that work:
- Elevate the affected arm on a pillow beside you to reduce nerve tension
- Use an over-the-door cervical traction device for 10 to 15 minutes before bed
- Apply ice to the neck for 15 minutes before lying down
- Do scapular retractions before sleep — squeeze shoulder blades together, hold 5 seconds, repeat 10 times
Cervical Radiculopathy Exercises: What to Do (and What to Skip)
Up to 90% of cervical radiculopathy cases can improve with conservative treatments, including physical therapy and exercise. The key is doing the right moves and avoiding the wrong ones.
Chin Tucks
Lie on your back, tuck your chin as you gently press your head back into the surface without moving your chin up or down, hold for 5 seconds, then relax. Complete 10 to 15 repetitions. This is the foundational exercise for cervical radiculopathy — it strengthens the deep neck flexors that stabilize your cervical spine and reduce nerve root pressure.
Shoulder Blade Squeezes
Stand or sit tall. Squeeze your shoulder blades together firmly, hold for 10 seconds, release. Repeat 5 times. This exercise targets the postural muscles that support upper back comfort and indirectly reduces cervical nerve tension.
Neck Side Stretches
Gently lower your left ear toward your left shoulder. Use your hand to add very gentle downward pressure — never force it. Hold for 20 seconds. Repeat on the other side. Do 3 to 5 repetitions per side. This builds flexibility and reduces nerve irritation over time.
Shoulder Rolls
From a relaxed standing position, circle your shoulders forward 5 times, then backward 5 times. Repeat throughout the day. This dissolves shoulder tension that often contributes to cervical nerve compression.
Neck Extensions
Lie face down with your head just beyond the edge of a bed. Slowly lower your head toward the floor and hold for approximately one minute. This gently creates space between cervical vertebrae. Stop immediately if arm symptoms intensify.
What NOT to do with cervical radiculopathy:
Avoid heavy overhead lifting, breaststroke swimming (it locks the neck into extension), sudden forceful head rotations, sit-ups or crunches (they spike spinal load), and any movement that makes arm symptoms worse. In the early stages, avoid strenuous activities such as heavy lifting and excessive reaching with the affected arm, and avoid activities that tip the head backward or sideways for extended periods.
2026 Updates: What Is New for M54.12 This Year
Here is what every provider and coder needs to know right now:
M54.12 remains valid and billable with no structural changes in the 2026 ICD-10-CM edition.
AI documentation tools are now mainstream. Many practices use AI in 2026 to suggest ICD-10 codes from clinical notes. These tools are helpful but imperfect — they still regularly confuse M54.12 with M50.1x or suggest unspecified codes when specific ones apply. Always verify every AI-generated code before submitting.
Payer audits on radiculopathy codes have increased in 2026. Claims pairing M54.12 with high-complexity E/M codes (99214 or 99215) are drawing more scrutiny. Your documentation of medical decision-making needs to clearly justify the complexity level selected.
Telehealth is now accepted for cervical radiculopathy by most major payers, but documentation requirements are unchanged. The exam findings, clinical reasoning, and symptom details must still appear in the note even for virtual visits.
Medicare acupuncture continues to require M54.50 or M54.59 — not M54.12. If a patient presents with both low back pain and cervical radiculopathy and is seeking acupuncture coverage, the acupuncture service must be billed under the appropriate low-back code.
MS-DRG v43.0 is the current grouper for M54.12, placing it under DRG 073 (with MCC) and DRG 074 (without MCC). Inpatient coders should verify secondary diagnoses that may affect the MCC/CC determination and DRG assignment.
Frequently Asked Questions About M54.12
What is M54.12? M54.12 is the ICD-10-CM diagnosis code for Radiculopathy, Cervical Region. It is a billable/specific code used to denote radiculopathy specifically located in the cervical area of the spine, involving nerve pain caused by compression or irritation of cervical nerves.
Is M54.12 the same as a pinched nerve in the neck? Yes, essentially. Cervical radiculopathy — what M54.12 documents — is the clinical term for what most people casually call a pinched nerve in the neck.
Can I bill M54.50 and M54.12 together? Yes, when both conditions are separately documented and clinically supported. There is no Excludes 1 restriction between M54.50 (low back pain) and M54.12 (cervical radiculopathy). Verify with your specific payer.
Can M54.12 and M50.1x be billed together? No. If a confirmed cervical disc disorder is causing the radiculopathy, you must use M50.1x — a combination code that replaces M54.12. Using both together violates Excludes 1 rules.
What exercises are safe for cervical radiculopathy? Chin tucks, scapular retractions, gentle neck side stretches, and shoulder rolls are safe and effective. Exercise treatments for cervical radiculopathy typically involve deep cervical flexor muscle training, posture correction, and muscle stretching, and appear to improve body structure, function, and patient participation in daily activities.
How long does cervical radiculopathy take to heal? Most cases improve within 4 to 6 weeks with conservative management. According to the Journal of the American Academy of Orthopaedic Surgeons, up to 75% of cases of acute cervical radiculopathy improve spontaneously, which is why nonsurgical treatment is always tried first.
What should you not do with cervical radiculopathy? Avoid stomach sleeping, heavy overhead lifting, breaststroke swimming, sudden forced neck movements, and any exercise that worsens arm symptoms. Prolonged forward head posture from screen use is also a major aggravator to eliminate.
Is M54.12 valid in 2026? Yes. M54.12 is valid for the submission of HIPAA-covered transactions from October 1, 2025 through September 30, 2026.
Final Thoughts
Whether you are a coder trying to get claims paid cleanly, a provider documenting a complex patient visit, or a patient who just found out they have cervical radiculopathy — understanding M54.12 gives you a serious advantage.
This code is not complicated once you know what it represents: a pinched or irritated nerve root in the neck, producing real symptoms that deserve both precise clinical attention and accurate documentation. Use it correctly, document thoroughly, respect the Excludes 1 rules, and keep the patient’s recovery at the center of everything you do. That is how you win at good medicine and clean billing in 2026.
This article is written for educational and informational purposes only. Always consult a licensed medical coder, billing specialist, or qualified healthcare provider for advice specific to your clinical or coding situation.