If you work in cardiology billing, internal medicine, or any hospital coding department, the CHF exacerbation ICD-10 code is something you deal with almost every single day. And yet it trips up even experienced coders. Use the wrong code, and you are looking at claim denials, audit flags, and reimbursement delays that eat straight into your revenue cycle.
So let’s break it all down, plain and simple, so you walk away knowing exactly which code to use, when to use it, and how to document it right the first time.
What Is CHF Exacerbation? (And Why the ICD-10 Code Matters So Much)
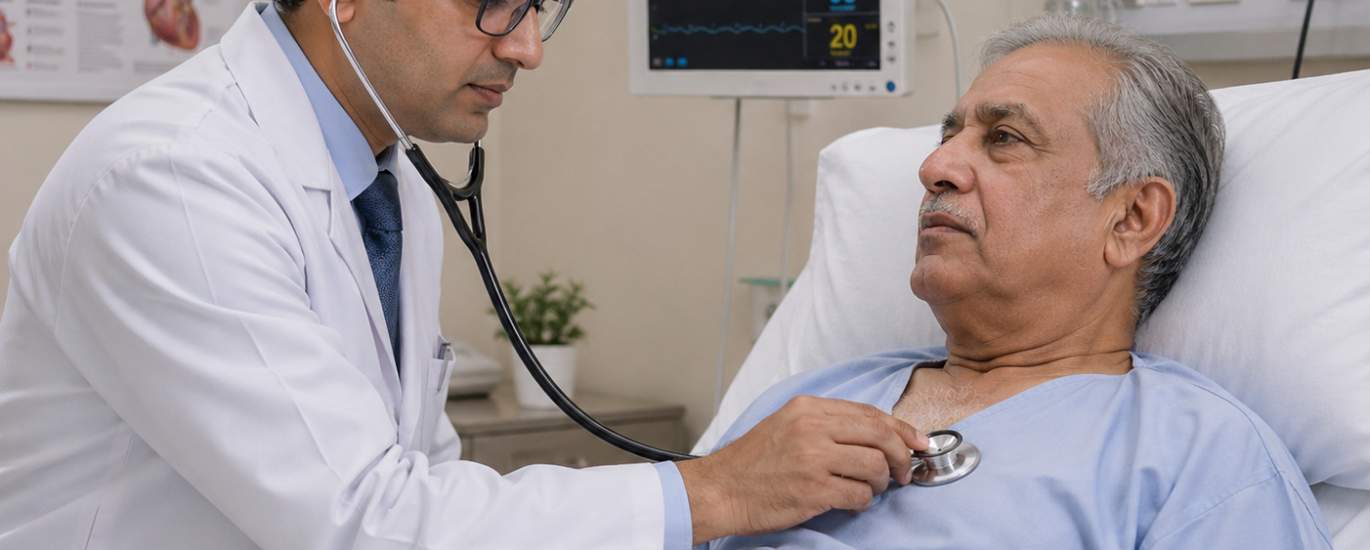
Congestive heart failure (CHF) exacerbation happens when a patient’s already-existing heart failure suddenly gets worse. The heart, which is already struggling to pump blood effectively, takes a hit from a trigger and decompensates. The result is a rapid worsening of symptoms that often lands the patient in the ER or earns them a hospital admission.
Now, here is where ICD-10 coding comes in. The icd 10 code for chf exacerbation is not just a billing checkbox. It tells insurers, auditors, and CMS exactly what type of heart failure is happening, how severe it is, and whether it is a new event or a flare-up on top of a chronic condition. Get that specificity right, and you get paid correctly. Get it wrong, and the claim bounces.
The 2026 ICD-10-CM edition, which became effective on October 1, 2025, and stays valid through September 30, 2026, puts even stronger pressure on coders to document with precision. Vague entries like plain “CHF” or I50.9 without clinical support are red flags for payers and auditors alike.
The Core CHF Exacerbation ICD-10 Codes for 2026
Before diving into the details, here is your quick-reference breakdown of the most commonly used CHF exacerbation codes under the I50 category:
I50.9 – Heart Failure, Unspecified This is the catch-all code. Use it only when documentation does not specify the type or acuity. It is billable, but it often results in lower reimbursement. Think of I50.9 as your last resort, not your go-to.
I50.21 – Acute Systolic (Congestive) Heart Failure Use this when a brand-new systolic failure hits and no prior chronic CHF is on record.
I50.22 – Chronic Systolic (Congestive) Heart Failure This is the icd 10 code for chronic systolic chf in patients who are stable, long-term systolic failure patients with ejection fraction (EF) under 40%.
I50.23 – Acute on Chronic Systolic (Congestive) Heart Failure This is the money code for exacerbation in a systolic CHF patient. When your chronic systolic CHF patient flares up, I50.23 is what you reach for. Documentation must show both the pre-existing systolic dysfunction and the new acute worsening. This is the most specific chronic systolic chf icd 10 code for exacerbation scenarios.
I50.33 – Acute on Chronic Diastolic (Congestive) Heart Failure Same concept as I50.23 but for diastolic dysfunction patients with EF at or above 50%.
I50.43 – Acute on Chronic Combined Systolic and Diastolic Heart Failure This is your chronic combined systolic and diastolic chf icd 10 code. Use it when a patient has both types of dysfunction documented and now presents with an acute flare. It is a fully billable 2026 code that requires documentation of both systolic and diastolic involvement, plus the acute exacerbation.
Symptoms of CHF Exacerbation
Knowing the symptoms helps coders push back on vague physician notes and request the specific documentation needed for accurate coding. During a CHF exacerbation, patients typically present with:
- Sudden or progressive shortness of breath (dyspnea), especially when lying flat (orthopnea)
- Rapid or unexplained weight gain, often several pounds over a few days
- Swelling in the legs, ankles, or abdomen (edema and ascites)
- Fatigue and reduced tolerance for any physical activity
- Persistent cough, sometimes with foamy or pink-tinged mucus
- Rapid or irregular heartbeat (palpitations)
- Reduced urine output despite fluid buildup
- Mental confusion or difficulty concentrating in severe cases
Physicians should document all presenting symptoms alongside ejection fraction values and BNP or NT-proBNP lab results. BNP above 100 pg/mL or a clear elevation from the patient’s baseline strongly supports an exacerbation diagnosis.
Causes and Triggers of CHF Exacerbation
Understanding what causes a flare helps providers write stronger clinical narratives, which directly supports your coding and billing. Common triggers include:
Medication Non-Compliance – Patients who skip diuretics or other heart failure medications are the most frequent exacerbation cases. Documentation should note non-compliance directly.
High Sodium Intake – Dietary indiscretion is a classic culprit. A patient who overdoes it at a holiday dinner and shows up three days later with 10-pound weight gain and bilateral leg edema is a textbook case.
Respiratory Infections – Pneumonia, COVID-19, and even a bad flu can push a compensated CHF patient over the edge quickly. Code the infection as a secondary diagnosis when documented.
Uncontrolled Hypertension – Elevated blood pressure increases the workload on an already weak heart. When hypertension is documented alongside CHF, you must sequence correctly using I11.0 or I13.x depending on the clinical picture.
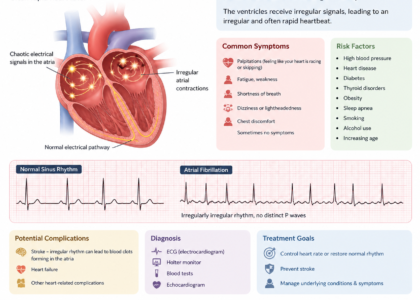
Cardiac Arrhythmias – Atrial fibrillation is a frequent companion diagnosis to CHF exacerbation. Rapid ventricular rate in AFib can directly trigger acute decompensation.
Fluid Overload – Sometimes from IV fluids in hospitalized patients or from renal disease preventing adequate fluid clearance.
Medication Side Effects or New Prescriptions – Certain NSAIDs, calcium channel blockers, and some diabetes drugs can worsen heart failure.
2026 Updates: What Changed and What You Need to Know Right Now
The 2026 ICD-10-CM edition became effective on October 1, 2025. While the core I50 codes themselves did not get major restructuring this cycle, the 2026 updates bring tightened documentation expectations and stronger emphasis on specificity across the board.
Here is what matters most for CHF coding in 2026:
Stronger specificity requirements. CMS and payer policies now treat generic documentation like “heart failure” or even “CHF exacerbation” without type specification as insufficient for high-level reimbursement. Physicians need to document systolic vs. diastolic, acute vs. chronic, and include measurable EF values.
Hypertension linkage is mandatory. The 2026 guidelines reinforce that when a patient has both hypertension and heart failure, coders must assume a causal relationship and use I11.0 (hypertensive heart disease with heart failure) rather than coding I10 and I50.x separately. Failing to do this is one of the top audit triggers in CHF claims.
End-stage heart failure gets its own add-on. When end-stage heart failure (I50.84) is documented, coders must add it alongside the primary type code. It is a “code also” instruction, not optional.
BNP and EF documentation now directly impacts risk adjustment. In value-based care models, accurate documentation of EF and biomarker values is tied to risk-adjustment scores. Practices with incomplete heart failure details see lower risk scores and lower payment rates.
CMS audit focus has not let up. CMS continues to flag heart failure claims with poor sequencing, missing linkage between hypertension and CHF, and use of non-specific codes where more specific ones are available.
Billing Tips for CHF Exacerbation: How to Get Paid Right
This section is where real money gets saved or lost. Follow these tips to keep your claims clean and reimbursements flowing:
Always specify the type. Before you even think about submitting a claim, the physician note must state whether the failure is systolic, diastolic, or combined. If the note just says “CHF,” query the provider before coding.
Document EF every time. Ejection fraction is the clinical anchor for distinguishing systolic from diastolic failure. An EF below 40% points to systolic (I50.2x). An EF at or above 50% points to diastolic (I50.3x). Values between 40 and 50 percent fall into a grey zone called HFmrEF and require careful provider documentation.
Use “acute on chronic” when applicable. If the patient has prior heart failure history and now presents with a worsening, I50.23, I50.33, or I50.43 is the right call, not the acute-only codes. This matters for DRG assignment and reimbursement level.
Sequence hypertension correctly. When hypertension is documented with heart failure, lead with I11.0 (hypertensive heart disease with heart failure), then add the specific I50.x code to identify the type. Reversing this order or coding them separately is a common compliance error.
Add secondary diagnoses. CHF rarely shows up alone. Code the trigger, whether that is atrial fibrillation (I48.x), pneumonia (J18.9 or more specific), CKD (N18.x), or fluid overload (E87.70). These secondary codes support medical necessity and can affect DRG grouping.
Include I50.84 for end-stage. If the physician documents end-stage heart failure, this code must accompany the primary type code. Leaving it out in an end-stage case is both a coding error and a missed reimbursement opportunity.
Link BNP results in documentation. Notes that reference BNP or NT-proBNP levels alongside symptoms and treatment plans are far more defensible in audits than narrative-only documentation.
Related Codes You Should Know
Working with CHF exacerbation means you will frequently encounter these companion codes:
| Code | Description |
|---|---|
| I11.0 | Hypertensive heart disease with heart failure |
| I13.0 | Hypertensive heart and CKD with heart failure, stage 1-4 |
| I13.2 | Hypertensive heart and CKD with heart failure, stage 5 or ESRD |
| I48.0 | Paroxysmal atrial fibrillation |
| I48.11 | Longstanding persistent atrial fibrillation |
| N18.3 – N18.6 | Chronic kidney disease stages 3 through 5 |
| E87.70 | Fluid overload, unspecified |
| I50.84 | End stage heart failure |
| Z87.39 | Personal history of other endocrine, nutritional, and metabolic diseases |
| Z79.899 | Long-term use of cardiac medications |
Always review the patient’s full medical history before finalizing code selection. CHF rarely exists in isolation.
Common Mistakes That Kill CHF Exacerbation Claims
These are the errors that coders make over and over, and every single one of them is avoidable:
Defaulting to I50.9 without querying the provider. I50.9 is unspecified heart failure. If the physician documented the type of heart failure anywhere in the encounter, you are obligated to use the more specific code. Using I50.9 when a better code exists is under-coding, and it costs you money.
Coding I50.21 and I50.22 separately when I50.23 applies. When a patient has both acute and chronic systolic heart failure documented, the correct code is I50.23, not two separate codes. This is a very common and very preventable error.
Not querying for EF when it is missing. If the note lacks EF documentation and does not specify systolic vs. diastolic, do not just guess. Send a query to the physician. This protects you from audit and gets the claim right.
Ignoring the hypertension linkage rule. Coding I10 and I50.22 separately when the patient has both hypertension and heart failure is wrong. The ICD-10-CM guidelines presume a causal relationship, and you must use I11.0 or I13.x instead.
Missing secondary diagnoses that affect DRG. Leaving out the AFib, the CKD, or the pneumonia that triggered the exacerbation can drop the patient into a lower-weighted DRG. Always code to the highest specificity the documentation supports.
Using acute codes for follow-up visits. Once the acute exacerbation has resolved and the patient is back to baseline chronic CHF, switch back to I50.22, I50.32, or I50.42. Using acute codes on outpatient follow-up visits is a red flag.
Frequently Asked Questions (FAQ)
What is the main ICD-10 code for CHF exacerbation?
The icd 10 code for chf exacerbation depends on the type of heart failure. Systolic CHF patients with an acute flare-up, use I50.23 (acute on chronic systolic heart failure). For diastolic, use I50.33. For combined, use I50.43. If the type is truly unspecified, I50.9 applies, but always try to get specificity from the provider first.
What is the ICD-10 code for chronic systolic CHF?
The icd 10 code for chronic systolic chf is I50.22. Use this for stable, ongoing systolic heart failure with EF under 40% when there is no current acute exacerbation.
What is the chronic combined systolic and diastolic CHF ICD-10 code?
For a stable patient with both types, use I50.42 (chronic combined systolic and diastolic heart failure). When that patient flares, switch to I50.43 (acute on chronic combined), which is the chronic combined systolic and diastolic chf icd 10 code for exacerbation scenarios.
Can I use I50.9 for CHF exacerbation?
Technically, yes, it is billable. But practically, you should only use I50.9 when the physician truly has not specified the type of failure and you cannot obtain clarification. Using I50.9 when better documentation exists is under-coding and may reduce reimbursement.
Do I need EF documentation to code systolic vs. diastolic CHF?
Yes. EF is the clinical gold standard for distinguishing these types. An EF below 40% supports systolic coding (I50.2x), while 50% or higher supports diastolic coding (I50.3x). Without EF, you need the physician to explicitly state the type in the documentation.
How do I code CHF exacerbation with hypertension?
When both hypertension and CHF are documented, use I11.0 as the primary code, then add the specific CHF type code (such as I50.23) as an additional code. Do not code them separately as I10 and I50.x.
What is the 2026 effective date for these CHF codes?
The 2026 ICD-10-CM edition became effective on October 1, 2025, and applies to all claims through September 30, 2026.
Does CHF exacerbation always require hospitalization to code the acute version?
No. Even in outpatient settings, if the physician documents an acute worsening of chronic CHF, the acute on chronic code applies. However, confirm that the documentation actually uses language like “acute exacerbation,” “decompensation,” or “acute on chronic.” Do not assume.
Final Takeaway
Mastering the chf exacerbation icd 10 coding landscape in 2026 is really about one thing: specificity. The days of dropping I50.9 on every heart failure visit and calling it done are long gone. Payers want type, acuity, ejection fraction, and supporting diagnoses. CMS wants correct sequencing and hypertension linkage. Auditors want documentation that tells the full clinical story.
When you get all of that right, you protect your practice from denials, boost reimbursement, and keep your revenue cycle healthy. When you get it wrong, the consequences show up fast, in the form of bounced claims, audit referrals, and clawbacks.
Use this guide as your daily reference. Query providers when documentation falls short. And stay on top of any mid-year updates CMS releases throughout the 2026 fiscal year, because in medical coding, staying current is not optional. It is the job.